From PPE to time for recharging, nurses have needed more
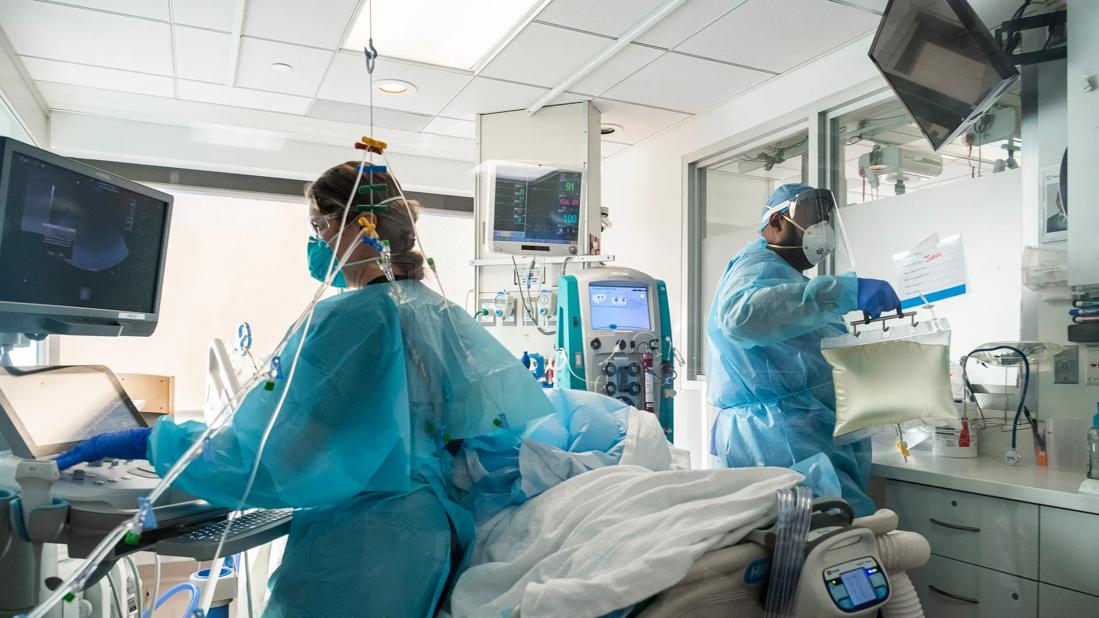
In the beginning of 2020, as the spread of SARS-CoV-2 sent families racing for dwindling supplies of bathroom tissue, nurses and other caregivers longed for another hard-to-come-by commodity: information about the virus itself. So much was unknown at that time.
Understanding of COVID-19 has vastly improved since then, but the pandemic continues to challenge nurses and other caregivers in myriad ways. The list of needs has ranged from the practical, such as disposable masks, gloves and gowns, to the personal, including support for mental and emotional health.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Acknowledging which resources nurses needed during the crisis offers insights into how some problems were solved and illuminates opportunities for improvement as healthcare leaders prepare for the future.
In a published report that addressed nurses’ resiliency during the surge in the spring of 2020, the authors noted that the global shortage of personal protective equipment (PPE) created extensive stress for nurses, who wondered how they would protect themselves and their patients.
At Cleveland Clinic, supply chain leaders leaned on relationships inside and outside the health system to create source redundancy in a variety of ways. As an example, the healthcare system developed a process for sterilizing N95 masks so that they could be safely reused.
Maureen Schaupp, MSN, APRN-CNP, CHFN, Associate Chief Nursing Officer for Advanced Practice Nursing and Nursing Quality and Practice, says that during the PPE crisis, nurses needed two things: supplies and assurances.
“They needed frequent and timely communication about supplies, and they received that at Cleveland Clinic. The messaging that we had enough PPE calmed many nurses,” Schaupp says.
Cleveland Clinic also established a COVID-19 hotline for caregivers who were concerned they might have contracted the virus, as well as a toolkit containing up-to-date resources for “Coping in Times of Uncertainty.”
Communications technology such as computer tablets quickly became essential as restrictions on visitors, aimed at minimizing risk of transmission of the virus, resulted in bedside nurses becoming the primary contact for hospitalized patients. The ability of patients to have video chats with loved ones ameliorated some of the isolation that amplified suffering. Early hurdles included assisting families with enabling their own devices to allow digital connections to be made.
Advertisement
It could take up to 45 minutes to help a family member prepare for a virtual call with a patient, says Nelita Iuppa, DNP, MS, NEA-BC Associate Chief, Nursing Officer, Informatics. Cleveland Clinic’s Office of Patient Experience provided that help to families, which allowed nurses to stay focused on bedside care.
For nurses accustomed to evidence-based practice standards, the mysteries of COVID-19 proved especially vexing. In the resiliency report discussed earlier, the authors learned that negative emotions nurses experienced were associated with a lack of evidence-based practice recommendations for caring for patients with COVID-19.
Evidence gathered over weeks and months helped hone best practices. Early prone positioning for awake patients with severe respiratory distress due to COVID-19 emerged as a best practice. A novel virus, Schaupp notes, can create an environment where nurses must do what they do best: adapt as information accrues.
“Long-standing evidence can be a rare luxury,” Schaupp says. “In the first months of the pandemic, everyone was trying their hardest, and we were learning all the time. We had to pivot many times a day. When a change in protocol came about, a key factor in implementation was that we explained why we were making it.”
As the pandemic stretched on, the tidal wave of donations of food and public thank-yous waned, yet nursing teams continued to work harder than ever. A nationwide nursing shortage, worsened by the pandemic, added to nurses’ work stress.
At Cleveland Clinic, leaders made an early commitment to maintain its workforce when other institutions were issuing temporary layoffs. Cleveland Clinic caregivers were recognized with a one-time bonus, a gift of gratitude for their efforts during the crisis.
In the end, Schaupp says, what most nurses seem to want is more nursing caregivers. “They want more help,” she says. Cleveland Clinic has expanded nursing recruitment efforts, says Kiersten Kanaley, Executive Director of Talent Acquisition Operations.
“To meet nurses where they are, we are engaging with them through digital media campaigns, campus recruiting events, virtual events and a newly redesigned careers website,” Kanaley says. “A new sourcing team that identifies and engages talent through proactive recruiting techniques, similar to agency recruitment, is activating in November. Early next year, we are introducing interviewing technology with candidate self-scheduling and realistic job previews.”
Advertisement
In addition to cross-training to meet clinical needs during patient surges, nurses need support from other nurses and from hospital systems to manage the unique pressures of the pandemic world. Cleveland Clinic’s Caring for Caregivers program helps employees by making confidential, no-cost counseling available for family and emotional problems, substance use, financial challenges, and loss and bereavement. The health system also connects caregivers to resources for child care and elder care.
With two years of pandemic response under their belts, nurses at every level have been part of creating a future where their needs are being met. Relationships and teams that have been strengthened through collaboratively searching for solutions will serve nursing caregivers as they adapt and face tomorrow’s challenges.
Advertisement
Advertisement

Planning continues with critical, patient-focused input from nursing teams

Strengthening care through targeted resources and frontline voices

Embracing generational differences to create strong nursing teams

CRNA careers offer challenge and reward

An unexpected health scare provides a potent reminder of what patients need most from their caregivers

Cleveland Clinic Abu Dhabi initiative reduces ICU admissions and strengthens caregiver collaboration

Veteran nurse blends compassion, cutting-edge transplant training and military tradition to elevate patient care

Embrace coaching and other tips to be a stronger leader