A high-level of expertise with a versatile technique is leading to reduced complications and easier post-operative recovery for patients
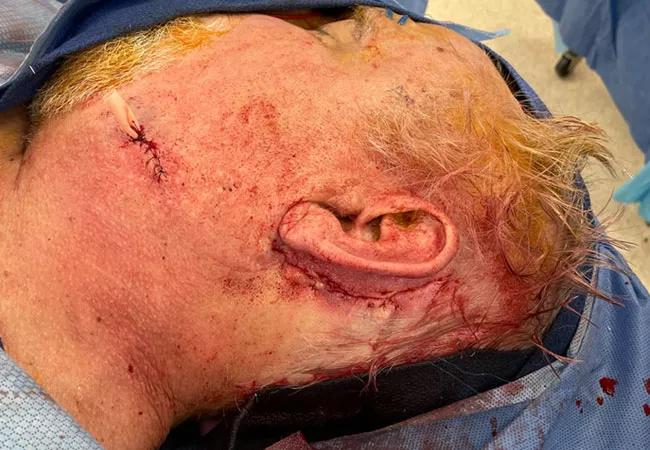
Patients with complex scalp and cranial vault defects can present a unique challenge for reconstructive surgeons. The three primary reconstructive goals are to protect the underlying brain, separate and seal-off the subdural space, and recreate the natural contour of the skull and scalp to ameliorate disfiguring deformity. Cleveland Clinic’s Head & Neck Institute will see patients with defects of the scalp and/or cranial vault for a variety of reasons including trauma, previous neurosurgical procedures or various cancers.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Many patients present to Cleveland Clinic after having had multiple surgeries and/or radiation to the region. In this setting, the tissue quality of the remaining scalp can be poor. It is oftentimes scarred, contracted and has poor vascularity. Attempts to place rigid implants, such a titanium under a compromised scalp, can lead to wound break down, implant extrusion and the need for further operations.
Surgeons within Cleveland Clinic’s Head & Neck Institute have taken on a new approach to address this difficult clinical problem and are seeing promising results. “We have been able to help patients with longstanding deformities that have often lost hope of ever having a normal appearance and contour to their skull,” says Peter Ciolek, MD, one of the facial plastic and reconstructive surgeons at the institute. “The key element in our technique is the use of the anterolateral thigh (ALT) free flap. This allows us to transplant highly vascularized tissue to the recipient site to support and protect any necessary alloplastic implants.”
Dr. Ciolek, along with Michael Fritz, MD, the section head of facial, plastic and microvascular surgery, have developed expertise in the use of the ALT free flap for a variety of other clinical applications including the treatment of osteoradionecrosis, radical parotidectomy reconstruction, and hard palate fistulas.
The use of free flaps in cranioplasty and scalp reconstruction is not a new concept, but this technique offers several distinct advantages over more traditional methods. The relatively thin but robust fascia lata component is an ideal overlay for an alloplastic implant. Unlike muscle, the vascularized fascia lata does NOT lose its integrity, volume or contour overtime, which provides good long-term coverage and protection of implanted material. With more traditional techniques, such as the lattisumus dorsi free flap, the denervated muscle may thin overtime and lead to delayed implant exposure and infection.
Advertisement
The vascularized fascia lata can also be used as a dura overlay in cases of cerebrospinal fluid leak. Non-vascularized fascia lata has been used extensively for repair of cerebrospinal fluid leaks in anterior skull base surgery. “We have found it to be equally effective in its applications to cranioplasty. The fascia lata component of the free flap can be directly sewn to the edges of torn dura or can act as an overlay after dural repair with another material,” says Dr. Fritz. Once healed, this can act as durable, water-tight barrier that will not thin or atrophy, like what has been observed with myocutaneous free flaps.
“We have found the ALT to be amazingly versatile in the reestablishment of skull and scalp contour. Through the implementation of perforator harvest techniques, the ALT can be sculpted and contoured to each individual patient. If the thickness of the fasciocutaneous ALT does not match the desired thickness of the reconstruction, the flap is performed as an adipofascial flap with a skin graft,” says Dr. Ciolek.
Traditionally, rigid alloplastic implants are used to reestablish contour. Dr. Ciolek and the facial plastics team have found that trying to match the contour with a rigid alloplastic implant can often lead to a large amount of dead space between the implant and the underlying scarred dura. “If the dead space is left to remain, this will frequently lead to breakdown of the overlying scalp and extrusion of the plate. Instead, we have taken the approach of achieving the final contour of the scalp by customizing the adiopofascial component of the flap which sits atop of the rigid alloplastic implant. While our method does provide rigid protection of the brain, it does not rely on alloplastic implants to completely restore the contour deformity. The subcutaneous fat of the AF-ALT can be sculpted to a precise contour and placed over the implant. Finally, if full scalp coverage cannot be obtained, a skin graft is placed on the smooth vascularized fascia or subcutaneous fat of the adipofascial anterolateral thigh free flap (AF-ALT), which is held in place by an aquaplast bolster,” says Dr. Fritz.
Advertisement
Even though free flaps are common-place in the world of head and neck reconstruction, they are still viewed as invasive and complex operations. The Cleveland Clinic Head & Neck microvascular team have been pioneers in the field of minimal access and low morbidity microvascular reconstruction. Dr. Ciolek explains that this has allowed them to reframe their approach to microvascular reconstruction to the point where they no longer consider this a highly invasive or radical procedure. “We have perfected our techniques in rapid identification of recipient site vessels using small, limited incisions,” he says. “In most cases, this avoids the need for large unsightly incisions on the neck. Secondly, because of our comfort and expertise in identification and use of the superficial temporal vessels, it avoids the need to vein grafting which can further complicate the microvascular portion of the procedure.”
In addition to minimizing morbidity at the recipient site, the team of surgeons have found the anterolateral thigh harvest site to offer little to no longer term consequences for the patient. Patients can expect to have full function and strength of their leg without the need for extended rehabilitation.
They have found that with this approach, they are able to safely discharge patients home much sooner than what was considered the safe standard. Following an uncomplicated surgery of this type, patients are ready for discharge on an average of three days, and some in as little as 24 hours.
Advertisement
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/9533eeab-1dc7-43a4-a3b0-1118bd2b558f/21-HNI-2148908-Cranioplasty-Scalp-Reconstruction-CQD_800x1200-inset-200x300_jpg)
These operations are often performed as a joint effort among the facial plastic and reconstructive surgeons or in conjunction with the neurosurgical team. While one surgeon performs exposure of the defect, customization of the rigid mesh plate, and identification of recipient site vessels, the other can harvest and prepare the AF-ALT. This cuts down significantly on operative time, which has been found to be an independent risk factor in operations such as this. Furthermore, collaboration in the operating room has lead to continued innovations in this technique.
Advertisement
Advertisement

Analysis of HNSCC patients shows HPV status to be predictive of higher abundance of oncobacteria within the tumor

Case study illustrates the potential of a dual-subspecialist approach

Evidence-based recommendations for balancing cancer control with quality of life

Study shows no negative impact for individuals with better contralateral ear performance

HNS device offers new solution for those struggling with CPAP

Patient with cerebral palsy undergoes life-saving tumor resection

Specialists are increasingly relying on otolaryngologists for evaluation and treatment of the complex condition

Detailed surgical process uncovers extensive middle ear damage causing severe pain and pressure.