Evidence-based therapies, monitoring, prevention and more

Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Management options for many of the vasculitic diseases have rapidly grown over the past 25 years. While novel treatment approaches represent important advances, the potential for relapse, treatment-related toxicity, permanent organ damage, and the emergence of other disease processes remain active issues that can result in morbidity or mortality. Because of these factors, optimizing care in people with vasculitis includes not only the selection of medications but other steps to detect or prevent future concerns.
The expansion of treatment options for vasculitis has raised many questions. Utilizing evidence-based therapeutic regimens provides the best means of approaching immunosuppression for these potentially life-threatening diseases. With the goal of providing guidance to healthcare providers, the American College of Rheumatology (ACR) and Vasculitis Foundation have recently published management guidelines for a number of the vasculitic diseases. 1-4
Monitoring is an essential part of care for people with vasculitis. Identification of active disease as early as possible may reduce the potential for organ damage. Monitoring also plays a critical role in detecting medication toxicity or the development of other diseases.
Regular physician visits represent the foundation of monitoring to assess the patient’s symptoms and signs. The frequency of visits will vary based on many factors, most significantly the recency of active disease or other acute issues. Regular laboratory monitoring is also critical. The typical labs I obtain include a complete blood count with differential, complete metabolic panel/chemistries (to include renal and hepatic studies and glucose), erythrocyte sedimentation rate and/or C-reactive protein, and a urinalysis in patients with any form of vasculitis that can affect the kidneys. How often labs are obtained will vary based on the medications the patient is receiving and where they are in their treatment course.
Advertisement
In people receiving cyclophosphamide or with recently active disease, I obtain labs every one to two weeks, with labs once a month in the setting of other therapies. In patients with large vessel vasculitis, vascular imaging to look for new vascular lesions in new territories represents one of the main means of assessing for active disease.
Given that vasculitis is not only an inflammatory disease but one that affects the blood vessels, it is important to monitor lipids and blood pressure for cardiovascular health. This is particularly notable as some medications used in vasculitis can directly impact these modifiable parameters.
People with vasculitis remain at risk of the same health issues that can affect all people. At the time of their appointments, it is helpful to remind patients to keep up to date with health care screenings for the early detection of malignancy. As many immunosuppressive agents can increase the risk of skin cancers, regular skin checks by a dermatologist should be strongly encouraged.
Assertive use of available strategies that can minimize or prevent medication toxicities is important. Infection represents one of the greatest risks of the immunosuppressive agents used to treat vasculitis. Prophylaxis against Pneumocystis pneumonia should be given to patients receiving regimens known to place patients at increased risk of this opportunistic infection. Use of non-live vaccines represents another means of lessening preventable infections.
Some medications have toxicities for which an effective prevention strategy exists. Examples include taking daily oral cyclophosphamide in the morning with a large amount of fluid to prevent urothelial toxicity or the use of folic acid with methotrexate. A recently updated ACR guideline for the prevention and treatment of glucocorticoid-induced osteoporosis was presented at ACR Convergence 2022.
Advertisement
Reproductive health risks from medication and underlying disease also need to be recognized in people with vasculitis. In young women, discussions about the need for preconception planning to optimize pregnancy safety for both mother and child should start at an early point following diagnosis. Use of medications that impact fertility or that carry teratogenic potential must be weighed carefully, with application of risk mitigation strategies when these agents are required to treat vasculitis.
Determining whether new symptoms, signs, laboratory, and/or imaging findings are indicative of active vasculitis can be very difficult. Particularly in immunosuppressed patients, the possibility that a new or persistent feature could represent something other than vasculitis must always be considered. Permanent damage, infection, medication toxicity or another medical diagnoses can all have similar presentations to what can be seen with active vasculitis. How to differentiate these will vary depending on the presenting features, but recognition of this potential is an essential first step in this process.
Educating the patient and their family about vasculitis and the medications used to treat it begins on the first encounter and continues during each visit thereafter. Facing the uncertainty of what lies ahead when confronted by a medical illness is a challenge shared by all people. Knowledge is empowering, and regular discussion of factors we understand and can control provides a means of combating such uncertainty. These discussions also provide a valuable tool in understanding the patient’s concerns and priorities that can help to guide management through shared decision making now and in the future.
Advertisement
1. Gorelik M, et al. 2021 American College of Rheumatology/Vasculitis Foundation Guideline for the Management of Kawasaki Disease. Arthritis Rheumatol. 2022 Apr;74(4):586-596.
2. Maz M, et al. 2021 American College of Rheumatology/Vasculitis Foundation Guideline for the Management of Giant Cell Arteritis and Takayasu Arteritis. Arthritis Rheumatol. 2021 Aug;73(8):1349-1365.
3. Chung SA, et al. 2021 American College of Rheumatology/Vasculitis Foundation Guideline for the Management of Antineutrophil Cytoplasmic Antibody-Associated Vasculitis. Arthritis Rheumatol. 2021 Aug;73(8):1366-1383.
4. Chung SA, et al. 2021 American College of Rheumatology/Vasculitis Foundation Guideline for the Management of Polyarteritis Nodosa. Arthritis Rheumatol. 2021 Aug;73(8):1384-1393.
Advertisement
Advertisement
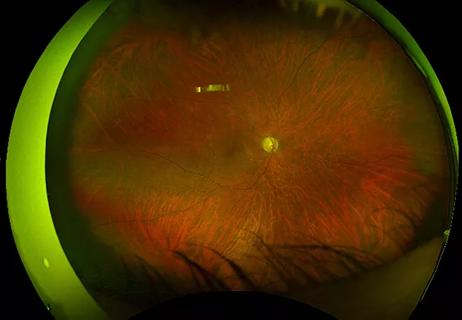
Holistic approach is necessary to ensure a correct diagnosis
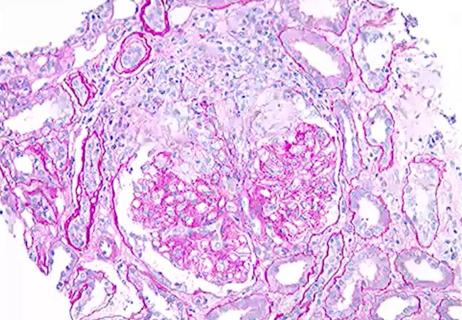
Knowing the affected organs and vessels can help in identifying cause

Unraveling the TNFA receptor 2/dendritic cell axis

Nasal bridge inflammation, ear swelling and neck stiffness narrow the differential diagnosis

Genetic testing at Cleveland Clinic provided patient with an updated diagnosis
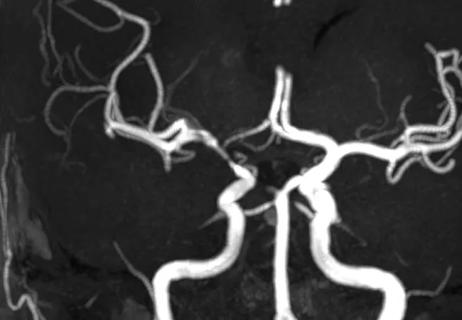
Combining quantitative vessel wall MRI metrics, CSF abnormalities and neurologic symptoms can be highly predictive

From dryness to diagnosis

Multiple comorbidities are associated with pediatric psoriasis