Strengthening outcomes through clear, transparent communication
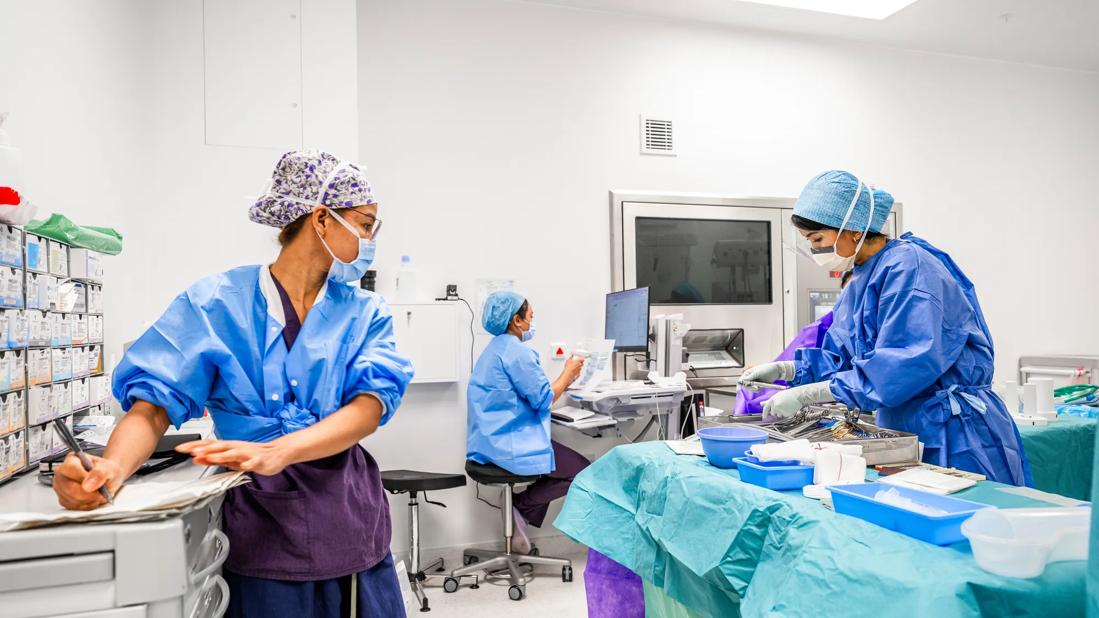
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/9a7190cd-458e-49ed-bc38-918da617423d/CCC_5210909_09-05-24_0969_MLC)
Nurses in surgery
In today’s complex surgical environment, effective communication and cohesive teamwork remain the strongest safeguards against medical errors and poor patient outcomes. As perioperative care becomes increasingly sophisticated, the role of the Registered Nurse First Assistant (RNFA) has evolved beyond technical expertise into visible, everyday clinical leadership.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
To better equip RNFAs for the realities of modern surgical practice, Cleveland Clinic has developed a new onboarding process focused not only on technical skill development, but also on advanced communication strategies and the critical role first assistants play as leaders, educators, patient advocates and collaborative team members.
For healthcare professionals working in and around the operating room (OR), strengthening communication and team dynamics is not optional — it is foundational to safe surgical care, explains Ashlee Cummings, BSN, RN, CNOR, CRNFA, who helped design the curriculum. Cummings, one of the Lead Surgical Clinician Educators for the Department of Thoracic and Cardiovascular Surgery at the Cleveland Clinic, first shared the concept in a presentation, The RNFA Leader: Patient Safety Starts and Ends with You, at the Association of PeriOperative Registered Nurses (AORN) Global Surgical Conference and Expo in 2025.
“With steady job growth projected over the next decade, RNFAs aren’t just expanding in number, we are expanding in influence, shaping the future of surgical quality and patient outcomes,” Cummings says. “But technical skill alone doesn’t guarantee safety in the OR. How we communicate, particularly under pressure, can directly impact patient outcomes. That’s why we created this program. We want RNFAs to feel confident working with their hands and also in using their voices.”
Cummings emphasizes that communication in the OR requires more than clear speech. It is a dynamic exchange that requires listening, observing and interpreting both verbal and nonverbal cues.
Advertisement
"The orientation process teaches that effective exchanges are grounded in high-quality communication," she explains. "Small misunderstandings can escalate quickly in a high-stakes environment. An assumption that goes unclarified or a rushed handoff may seem minor, but those gaps can compound into real safety concerns.”
To minimize risk, Cummings encourages teams to use standardized communication tools such as SBAR and the Universal Protocol within their workflows, particularly during surgical time-outs and critical intraoperative events.
“Finetuning our communication skills is a continuous process, but it’s one of the most powerful tools we have for reducing harm, improving efficiency and enhancing the patient experience," she says. "Clear, concise communication doesn’t just elevate performance, it can save lives.”
Cummings adds that communication frameworks like TeamSTEPPS, closed-loop communication and structured conflict resolution strategies can be adopted across hospitals and health systems to promote safer, more collaborative operating environments.
“These skills strengthen clinical effectiveness — but just as importantly, they foster a culture of safety and mutual respect,” she says.
The clinician-led program also explores how cultural awareness and emotional intelligence shape interactions in the OR. Cummings stresses that eye contact, tone, proximity and phrasing can carry different meanings depending on cultural background.
“A culturally competent RNFA recognizes those nuances,” she says. “We adapt. We stay curious. And we approach every interaction with respect.”
Advertisement
Cummings also highlights the importance of reflective practice.
“Retrospection and introspection help us grow,” she explains. “When we pause to evaluate our communication and our reactions, we strengthen our leadership.”
Transparency, psychological safety and trust are central themes of the course. The goal, Cummings says, is to encourage teams to use surgical checklists, open reporting systems and post-case debriefings to reinforce these principles and ensure that every team member feels safe speaking up.
Conflict in the OR is unavoidable, particularly in high-pressure settings where goals, resources or responsibilities may seem misaligned, Cummings notes. To address these potential tensions, the RNFA onboarding program teaches a structured conflict management approach that includes:
“Professionalism is our first line of defense,” Cummings explains. “As RNFAs, we set the tone. When we model accountability and respectful dialogue, it changes the dynamic for the entire team.”
She adds that clarity from the outset can make a measurable difference: “When teams openly share objectives and define roles at the beginning of a case, we see fewer downstream disruptions."
Research shows that clinicians under stress are more prone to technical errors, reinforcing the need for strong, supportive team dynamics. Cummings adds that high-performing surgical teams share several common traits: trust, accountability, adaptability, clear goals, adequate resources and a commitment to continuous learning.
Advertisement
“These aren’t abstract ideas,” she says. “They’re behaviors we practice every day: leadership, mutual support, situational awareness and structured communication. When those elements are present, the OR becomes safer for everyone.”
Ultimately, Cummings believes RNFA leaders do far more than assist in the surgical field. As healthcare systems face staffing challenges, rapid onboarding and heightened interdisciplinary complexity, she stresses that strong communicators are becoming increasingly essential.
"Leadership in the OR isn’t static," she notes. "It requires reflection, adaptability and deliberate practice. Our goal is to support healthcare professionals across disciplines so that safe patient care isn’t just an aspiration, it’s a lived reality.”
Advertisement
Advertisement
How meaningful relationships, psychological safety and everyday recognition can help sustain caregivers
Veteran nurse shares how perseverance and support can fuel impactful ideas
Interdisciplinary initiative leverages technology, documentation and diagnostic clarity to prevent skin breakdown
Program helps caregivers prepare for the unique pressures of the ICU
Multidisciplinary simulations provide realistic emergency training to help achieve optimal patient outcomes
How critical care expertise, rapid decision-making and patient advocacy are shaping perioperative care
Survey identifies opportunities for further training and ongoing moral support
Nursing quality experts help drive policies and practices designed to meet the highest clinical standards