Pediatric survival rates from sudden cardiac arrest are abysmal
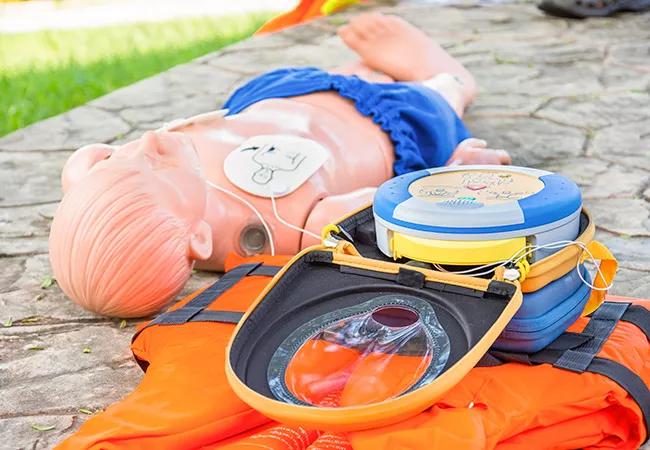
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/56592a19-f743-445d-9f04-a0973381da7c/GettyImages-617377094_jpg)
GettyImages-617377094
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Alec Kornet traveled directly from baseball conditioning to hockey practice the evening he passed away. Alec also played baseball, was a drummer in the high school marching band and was an honors student. Alec’s mother says she had no indication that the 17-year-old high-school junior had a heart condition – in fact, he had passed his annual physical months before.
When Alec took the bench because he wasn’t feeling well, he told his brother, then-sophomore Mike Kornet, who was playing goalie at the time, that he was feeling light headed. Alec crawled off the ice and collapsed on the bench, where he received CPR until paramedics arrived. He did not respond to resuscitation efforts, and passed away that evening at the hospital.
Tragic stories like Alec’s are fortunately rare; however while sudden cardiac arrest is certainly not as common in pediatric patients as it is in adults, it certainly does happen. In those circumstances, just about the only thing that may save that child’s life is an automated external defibrillator (AED).
We conducted a study to get a better sense of how factors like age and neighborhood characteristics, including racial composition and median household income, impact AED application before the arrival of emergency medical services (EMS). In our analysis of prospectively collected data from the Cardiac Arrest Registry to Enhance Survival (CARES), we identified just under 1,400 patients who had cardiac arrests between the ages of 1 and 18. Unfortunately, AEDs were applied to only 28% of these patients prior to EMS arrival. Multivariate analysis indicated that age was the most powerful predictor of AED application, regardless of race, sex, location or neighborhood characteristics. Older patients (12 – 18 years) were 1.4 times more likely to have AEDs applied than patients who were 11 years-old or younger.
Advertisement
Only 19% of this group of 1,398 young patients with cardiac arrest survived to hospital discharge.
Clearly, there’s work to do here. We see automated external defibrillators (AEDs) out there in the community, at sports facilities and shopping centers; however, the abysmal survival rates suggest that people are not using them.
The low rate of AED application is likely multi-factorial. The community members may assume that the child is experiencing respiratory distress rather than cardiac arrest. We also think there is concern about using devices on children that were intended for use on adults. Community members may worry about causing harm. But, from a caregiver’s perspective, there’s no harm more significant than sudden death.
Although some AEDs come with child-sized pads, the AED can still be used on young children and infants. Using pediatric pads is safer in that they reduce the amount of energy delivered thereby reducing injury (skin burns for example). However, when we’re dealing with a patient who has had a cardiac arrest, skin burns we can deal with. The loss of a child is always unacceptable.
Sometimes bystanders may worry that the victim is not in cardiac arrest, and that, by using an AED, they may put patients into cardiac arrest. But AEDs are by definition automated to tell users whether or not to shock. If you put an AED on somebody, and they’re having a seizure and their heart rhythm is okay, it’s not going to let you shock them or do anything harmful to the patient.
Advertisement
To be clear about this: there is no such thing as inappropriate AED use. In other words, if you think that you should be using an AED, use the AED.
The incidence of sudden cardiac arrest in children and adolescents is estimated between 0.5 and 2.0 per 100,000 person-years, with age-related variability in incidence and severity. Causes are not always identified, but include primary arrhythmias, myocarditis, cardiomyopathy and congenital heart disease. Autopsy showed that Alec died as a result of cardiomegaly, along with myocyte hypertrophy with hypergranular myocytes and epicarditis, findings suggestive of a heart muscle abnormality which likely led to a lethal cardiac arrhythmia.
Screening is a primary prevention tool, though clearly not perfect. Public awareness and availability of AEDs may be a more effective strategy as identifying all children at risk is not possible. In cases of witnessed sudden cardiac arrest, cardiopulmonary resuscitation (CPR) should begin promptly, followed by AED application as soon as it is available, with immediate CPR resumption.
Not long after Alec passed, his parents, Stephanie and Scott Kornet, began the 4Alec Foundation to raise awareness about sudden cardiac arrest and to educate first responders (i.e., athletic trainers, teaches, coaches and parents) in their community about the importance of prevention, as well as CPR and AED training.
Advertisement
Advertisement
Life-changing gene therapy is currently under FDA review
How evolving medical therapies and more precise patient selection are reshaping the role of intestinal transplantation
Cleveland Clinic specialist discusses the new clinical practice guideline
Introducing Prajwal Rajappa, MD, MS, Director of Pediatric Precision Oncology
The one-stop THRIVE clinic addresses renal, psychosocial, educational and other challenges alongside cardiac surveillance
Study found lower rates of nausea, vomiting and healthcare use through 12 months of follow-up
What to know about the condition, and 5 strategies to improve patient care
Biologic therapy and advances in monitoring may ease treatment and follow-up for families