Travel through time and see how the profession of nursing has evolved
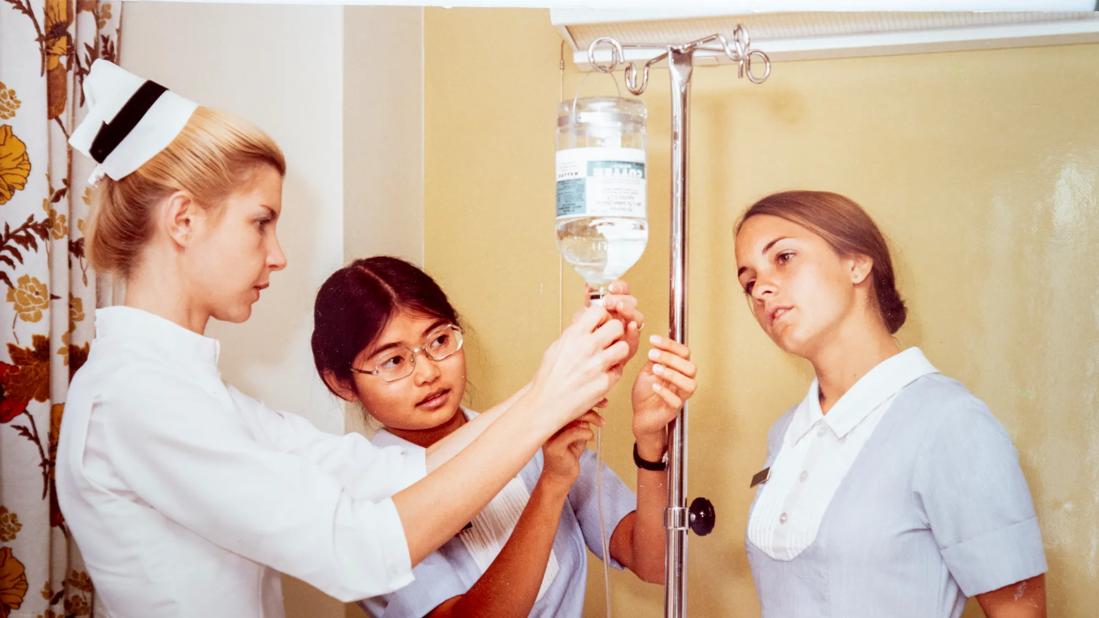
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/3f17730e-8220-4a9f-8190-c5bb1818a289/NUR_6199858_05-07-25_042_LDJ)
Cleveland Clinic nursing history
From Cleveland Clinic’s earliest days, nurses have been caring for patients at the highest level of skill, sharing their expertise with others and creating a brighter tomorrow in healthcare. They established the foundation for an extensive network of care, research and education that has evolved into today’s Stanley Shalom Zielony Institute for Nursing Excellence.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Much of the health system’s history has been built on the contributions of nurses to clinical operations, professional practice, patient care and the advancement of healthcare. As Cleveland Clinic celebrates its centennial anniversary, it also celebrates a century of nursing excellence. This visual showcase captures the spirit of the organization’s rich nursing history and offers a glimpse at the evolution of nursing at Cleveland Clinic.
Celebrating a Century of Nursing Excellence: Without Whose Aid, 3rd Edition will be released later this year. The book highlights the significance of nurses in making Cleveland Clinic one of the best healthcare systems in the world. The new edition includes a look at the last decade and the establishment of the Nursing Institute’s journey of integration within the health system.

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/922801ef-878d-4af4-816b-0c4783d27b72/1930s-1-1024x727_jpg)
1920s: Nurses line up in front of the original Cleveland Clinic hospital entrance on 90th Street in 1925. The hospital had seven floors and 184 beds. When this photo was taken, it employed 61 nurses, four postgraduate students, six female ward helpers and eight male orderlies.

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/c7e53faa-d8d9-466b-9b59-5952c1be8998/1930s-Neonatal-Ward-1_jpg)
1930s: By the late 1930s, hospital nursing staff switched from a nine-hour split shift to a straight eight-hour shift. The split shift, standard in U.S. hospitals at the time, had allowed nurses to cover service with two shifts a day. The change required the hospital to hire 25 new nurses. This photo from 1933 features neonatology nurses.

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/db832775-06c0-4aad-a00c-6ac138e25280/1940s-Nurses-Who-Remained-During-War_png)
1940s: In 1944, many nurses had left for military roles or defense-industry nursing. The remaining 50 who stayed at Cleveland Clinic performed a difficult and vital service. Outpatient visits and hospital admissions increased dramatically. The skill and dedication of nurses made it possible to keep the hospital up and running at 94%.
Advertisement

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/b2524294-116d-47dd-8d1a-28004362888e/1950s-nurses-training-as-tech-aides_png)
1950s: In 1958, the Cleveland Clinic Hospital Operating Room Department began training practical nurses as surgical technical aides. Graduates of the six-month program could fill the scrub nurse role under the supervision of a circulating nurse. Technical aides also cleaned and prepared instruments and equipment in the sterilizing room, and set up and cleaned patient rooms.
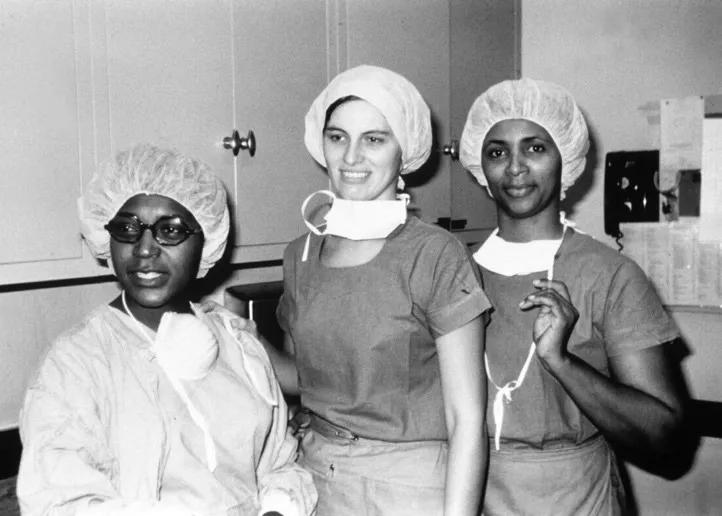
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/7f524c2f-2594-4876-9632-8b4ad1af478c/black-nurses_jpg)
1960s: Black nurses began to occupy administrative positions at Cleveland Clinic in the 1960s. Alma Davis was the first Black head nurse and later became a Clinical Director of Hospital Nursing. This photo shows another well-known nurse, Josephine Smith, RN (left), who served as head nurse in the operating room. Next to Smith are Linda Solar, RN (center) and Betty Williamson, RN.

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/c8fb1634-bff4-4ba0-a9f6-f897fc67ddb5/1970s-Nurse-anesthetists_png)
1970s: In 1970, Cleveland Clinic welcomed its first graduates from the School of Nurse Anesthesia. The Cleveland Clinic School of Nurse Anesthesia offered a two-year certificate program for graduate nurses.

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/b982e46c-021c-4ced-91ec-66a6b8489d62/1980s-research-and-education_jpg)
1980s: Research and education have always been pillars at Cleveland Clinic. This educational research poster on myasthenia gravis was developed by Angela Janik, RN (left). During the latter part of the 20th century many Cleveland Clinic nurses became established experts in clinical specialties, such as enterostomal therapy and wound and ostomy care. As professional nursing specialty organizations developed, Cleveland Clinic hosted many meetings, which included educational sessions.

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/df2769b8-0d46-4381-96b5-fb2033d31efc/1990s_jpg)
1990s: In the 1990s, nursing administrative structure and job descriptions changed. In 1992, head nurses became nurse managers, a change that acknowledged the responsibility of overseeing 50 or more employees as well as unit budgets and patients. In 1993, the same reform was carried out in ambulatory nursing. The patient care technician (PCT) position was also developed in the early 1990s. PCTs performed technical tasks along with the duties of nursing unit assistants, freeing RNs for assessment, care planning and patient education. This photo shows a licensed practical nurse with a patient.
Advertisement

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/f47c62d6-978a-4823-9277-e7f0146c346f/2000s-electronic-records-1_jpg)
2000s: In 2000, Cleveland Clinic transitioned from paper to the electronic medical record (EMR) system. Digital charting began in outpatient and ambulatory settings. By 2005, EMR was introduced in the first inpatient hospital setting and real-time nurse charting became standard. In 2006, wireless voice-over-internet-protocol phones were provided to staff to promote ease of communication. The same year, Cleveland Clinic launched its first high-tech nursing simulation lab to support the onboarding and education of new nursing staff.

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/d11a7dd1-854a-4467-bad4-d7096d4b5364/Magnet-1024x682_jpg)
2000s: Staying abreast of current technology helped in the considerable effort required to earn the American Nurses Credentialing Center’s coveted Magnet® recognition, the highest national recognition for nursing excellence, which was awarded to Cleveland Clinic’s main campus for the first time in 2003.

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/6e7dd0dc-7785-4748-9611-0ea6703195ae/19-NUR-5052-leadershipSummit-650x450-002_jpg)
2010s: Strategic planning at the Nursing Institute encompassed a layered approach to governance, including a strategic steering and execution team, decision-making team and affinity groups and operational teams. System-wide, nursing-specific communication was introduced, including a centralized nursing caregiver communications intranet page. In this photo, K. Kelly Hancock, DNP, RN, NE-BC, FAAN, who served as Executive Chief Nursing Officer from 2012 to 2020, is shown presenting at the annual Nursing Leadership Summit in 2019. The Nursing Institute presented its first Nursing Leadership Summit in 2009.

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/834813d2-f68e-4eca-9c14-27a8c3b7657b/18-NUR-859-Coyne-Hero-Image-650x450pxl_jpg)
2010s: The Nursing Institute implemented a continuous improvement process for the care of patients prone to falls, increasing nurses’ knowledge of HCAHPS and core measures, developed scorecards/metrics reporting, launched a leadership program for nurse management development, created a physician-nurse collaboration program and improved nursing informatics and information technology support of nursing practice. It established a Nursing Practice Council and outlined the first Professional Nursing Practice Model. In this photo, nurses are conducting purposeful hourly rounding, a project that launched in 2016.
Advertisement

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/d15886ed-a7f4-4b99-b801-1594277b7b0f/nurse-residency-690x380-650x358-1_jpg)
2010s: In 2014, the Nursing Institute launched Cleveland Clinic’s one-of-a-kind health system-based nurse residency, which offered a unique roadmap in aiding new nurses in the transition from academia to professional practice. It was designed to improve the practice readiness of new nurses to ensure a competent workforce and provide the enhanced training, skills and knowledge needed for new nurses to deliver superior, safe patient care.

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/08488e15-9e88-478a-bb70-94f18d1bba47/2010s-APRNS_jpg)
2010s: By 2016, with more than 1,000 advanced practice registered nurses (APRNs), Cleveland Clinic was the largest employer of APRNs in the state of Ohio, and one of the largest in the country. In September of 2016, Cleveland Clinic announced its first-ever ACNO of Advanced Practice Registered Nursing. With the creation of the position, the Nursing Institute standardized the reporting structure of all APRNs and physician assistants (PAs) in every institute and hospital.

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/bca3157b-6dfd-4434-ae82-25a6540eb32a/2020s-Nurses-Help-with-Testing-1024x569_png)
2020s: The Year of the Nurse and Midwife challenged nursing caregivers like never before while showcasing the true essence of the nursing profession. During the uncharted times of the pandemic, nurses’ hard work shined as a beacon of hope. Here, nurses are seen staffing the first COVID-19 testing site in the city of Cleveland.

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/ebc63916-7fa3-4168-8f10-2bc67ffce8c0/pitching-in-1_png)
2020s: Teams of Cleveland Clinic nurses and doctors volunteered to travel to areas that were hit the hardest by the pandemic, including New York City, Detroit and Abu Dhabi. They helped care for patients in hospitals that were overwhelmed with COVID-19 patients.
Advertisement

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/05067727-f9fe-4564-a621-115c713101cc/2020s-surge-hospital_png)
2020s: Nurses heeded the call to care for patients in unconventional spaces. This image shows Cleveland Clinic’s Hope Hospital, a 1,006-bed surge facility that was created in less than one month. As part of surge planning, nursing education leaders developed and launched an immersive clinical training experience for ambulatory and perioperative nurses, cross-training them to assist in critical and acute care settings, if needed. More than 4,100 nurses were cross-trained over the course of just a few weeks.
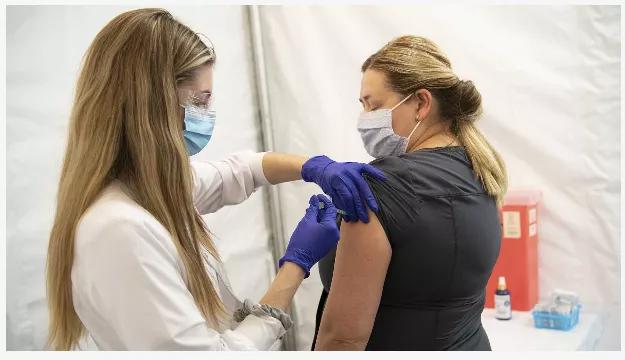
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/5e7b3866-e612-462c-bf14-2543fb27690a/2020s-giving-vaccine_png)
2020s: Cleveland Clinic nurses administered COVID-19 vaccines to caregivers and community members at one of the first vaccine sites to open.
Advertisement
Survey identifies opportunities for further training and ongoing moral support
Nursing quality experts help drive policies and practices designed to meet the highest clinical standards
Innovative workforce strategy transforms nursing careers through education, flexibility and ongoing support
Caregivers reflect on shared purpose, evolving practice and the enduring heart of the nursing profession
Nurse manager turns a patient safety concern into a data-driven effort to improve protocols and inspire innovation
Caregivers use targeted strategies to help patients move confidently and reduce the risk of injury
Perioperative educator shares insights into training the next generation of OR nurses
Expert nurses educate and support patients in managing diabetes for life