Multidisciplinary teams work together in in-situ scenarios
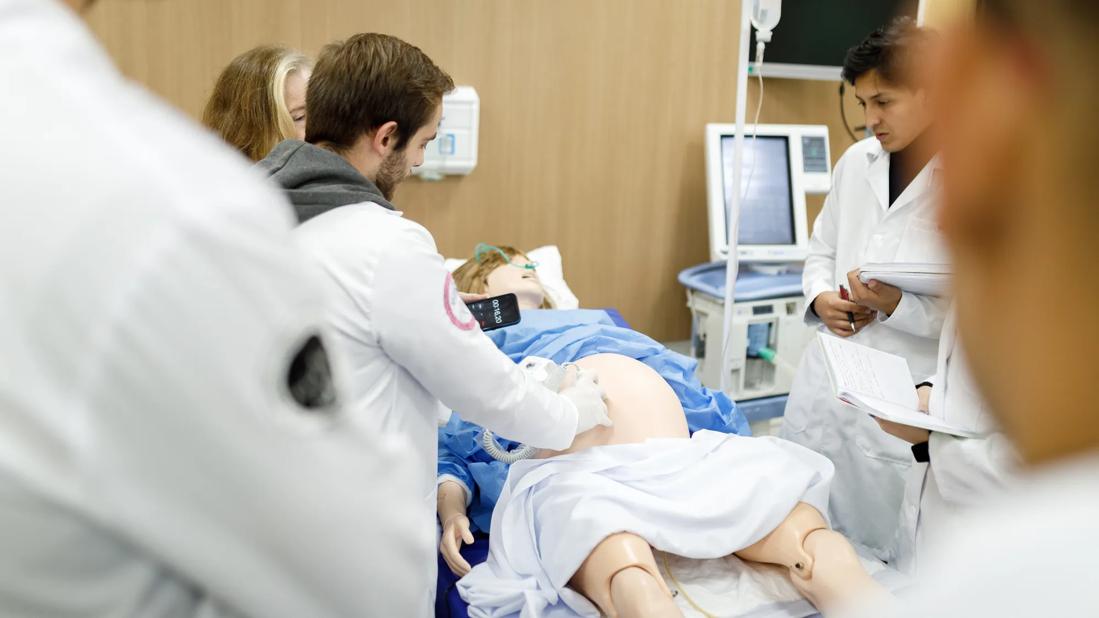
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/50320a91-ae74-4cfa-bec8-0cf8c8bf41ed/pregnancy-simulation-1502563306)
medical team surrounding a hospital bed with a "pregnant" medical manikin
The life-threatening peripartum complication amniotic fluid embolism (AFE) occurs once in every 40,000 deliveries in the United States. An obstetrician performing 100 deliveries annually has less than a 9% chance of encountering one over a 35-year career. Yet when an AFE happens, preparation is critical.
That’s why AFEs are among scenarios Erin Higgins, MD, includes in simulation training for Cleveland Clinic obstetrics teams. Dr. Higgins is Director of Simulation for the health system’s Obstetrics & Gynecology Institute, as well as Associate Medical Director of Cleveland Clinic’s Simulation and Advanced Skills Center, which is fully accredited by three simulation accreditation bodies. Over the last year, the center completed 5,687 events involving more than 75,000 learners.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Dr. Higgins develops curricula and runs simulation programs for a wide variety of learners and topics, including sharpening quality and safety practices among experienced teams.
An AFE is one example of a textbook HALO — high acuity, low occurrence event — for which preparedness is hard to come by. In the absence of direct experience, simulation training can provide familiarity to help prepare all members of a birthing patient's care team.
“We're able to practice these rare events so that the first time we're trying to manage them isn't with a real patient, it's with a manikin in a safe, controlled environment,” Dr. Higgins says.
Cleveland Clinic's Ob/Gyn simulation-based training emphasizes the importance of communication in addition to technical skills.
"Hospitals across the country do simulation training, but we're a big organization and we have hundreds of caregivers to train," says Dr. Higgins. "We include doctors, nurses, midwives, physician assistants, nurse practitioners and clinical-clerical associates. We involve the blood bank and anesthesia providers — it’s really the whole team, because on Labor and Delivery, it takes all these caregivers to manage a cardiac arrest or a massive postpartum hemorrhage."
Cleveland Clinic maternity caregivers are required to participate in these trainings every two years. Since 2022, more than 100 interprofessional simulation-based trainings have been held with more than 900 participants from 10 clinical backgrounds.
The simulation center is headquartered at Main Campus, but many sessions, including those in obstetrics, take place in situ, on hospital units. There, the simulation can reveal latent safety threats and allow teams to address potential problems such as with medication storage or equipment supplies.
Advertisement
High-fidelity pregnancy manikins are used to practice identifying and responding to conditions such as AFE, severe postpartum hemorrhage, resuscitative hysterotomy (formerly known as perimortem C-sections), pre-eclampsia, eclampsia and more.
Dr. Higgins starts the sessions with a pre-brief to orient learners to the session, followed by the hands-on scenario practice and a formal post-sim debrief.
Simulation standards recommend the debrief be two to three times the length of the practice scenario.
"For people who haven't done simulation-based training, there's often a misconception that the hands-on session is the 'cool' part," says Dr. Higgins. "And it is cool, but where we see the learning develop is really during the discussion afterward."
In addition to diving more deeply into details of the simulation, the debrief provides an opportunity to emphasize that every caregiver is empowered to ensure safety — a concept adopted by high-reliability organizations.
"Anybody can activate a code and get the people and resources," says Dr. Higgins. "We very much support 'if you see something, say something.' If you're uncomfortable, you can voice your concern."
As a passionate advocate for quality simulation training, Dr. Higgins frequently gives presentations on how to build robust Ob/Gyn simulation programs using guidelines embraced by the Society for Simulation in Healthcare. Quality simulation-based education requires so much more than manikins. It's about the entire experience, she says.
Advertisement
"You can do sim training in a good way or a bad way,” she says. “You can do it in a psychologically safe way or a psychologically unsafe way. We align our trainings with best practices to provide the optimal learning environment for our caregivers."
Old-school medical training approaches aren't helpful in the simulation environment.
"My colleagues put on a facilitator training the other day. During a discussion of how we talk to participants about the decisions they made, one of the participants raised their hand and asked, 'Where does shame come in?' That's how that person was trained," she says.
There may be simulation educators using shame in trainings, but that isn't best practice, she says.
"Simulation is a place for people to make mistakes, to try something that they're not sure about," Dr. Higgins says. "We make mistakes on the manikin so we don't make mistakes on patients. Creating a psychologically safe environment is key for learners to feel comfortable making mistakes. We don't trick people, there's no 'ha-ha, I got you.' The case scenario may not necessarily be easy and straightforward, because patients aren't always that way, but I'm not going to make you look stupid or call you out in the debrief. We're here to learn."
The Center for Medical Simulation at Harvard promotes a key tenet that Cleveland Clinic embraces, she says.
"The Basic Assumption© holds that everybody here is intelligent and capable, cares about doing their best and wants to improve. We may disagree from time to time, but everybody is here to take care of patients and to be the best caregiver they can be."
Advertisement
Advertisement
Data point to potential for targeted preconception planning
Reproductive psychiatry helps patients balance medication-related risks
Molecular Profiles Help Guide Referral and Care Planning
Hyperthermic intraperitoneal chemotherapy can improve patient outcomes
Leaning into therapies with the strongest evidence
A Q&A with Cleveland Clinic’s board-certified pediatric and adolescent gynecologist
Increasing uptake remains a challenge
Uterine transposition cleared the field for radiation therapy