Where sports medicine meets rheumatology
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Video content: This video is available to watch online.
View video online (https://www.youtube.com/embed/cR87BxMtvB0?feature=oembed)
Athletic Rheumatism: Former Gymnast with Low Back Pain
By Ahmed Elghawy, DO
In two recent cases, patients came to Cleveland Clinic with symptoms that were suspected to be associated with athletic activity. These cases underscore the fact that knowing how to differentiate a mechanical sports injury from a potential rheumatic disease that may require lifelong therapy can be the difference between disability and health.
A 20-year-old female has sought medical care at Cleveland Clinic’s Arthritis and Musculoskeletal Center for intermittent low back pain for 18 months. She is a former high school gymnast with a history of spondylolysis at age 16 from repetitive lumbar hyperextension injuries sustained during her floor routines. This had been treated conservatively, with complete resolution of symptoms.
Similar symptoms recurred 18 months ago, though this time without any known hyperextension injury, and were described as intermittent, achy, worse in the morning, and improved throughout the day and with naproxen (440 mg, twice a day as needed). One month after symptoms started, she was evaluated by her primary care physician, who ordered a lumbar radiograph that was reportedly unremarkable (per the patient) and was told that this was likely an exacerbation of her previous spondylolysis and advised to limit aggravating activities. She was referred to physical therapy for rehabilitation.
Unable to tolerate therapy at first, the patient was offered a muscle relaxant, which did not alleviate her symptoms. After completing eight weeks of therapy without relief, the patient slowly started to become more sedentary for fear of exacerbating her low back pain.
Advertisement
The patient reported that since this started, she has gained 40 pounds because of inactivity. Unable to tolerate performing her activities of daily living, she presented here for a second opinion. She had no known family history of autoimmunity.
Physical exam was significant for tenderness to palpation along the bilateral sacroiliac joints and right piriformis, without tenderness along the lumbar spine. A positive flexion abduction external rotation test was noted bilaterally, as was a Schober’s test with 4 cm.
Laboratory findings were significant for a positive HLA-B27 with normal sedimentation rate and C-reactive protein. Radiographs of the sacroiliac (SI) joints demonstrated sclerosis along the iliac margins of the SI joints, and MRI of the pelvis demonstrated evidence of active sacroiliitis. The patient was diagnosed with axial spondyloarthritis and was started on adalimumab 40 mg subcutaneously every two weeks. Upon re-evaluation at eight and 12 weeks, the patient’s low back pain had resolved, and she was performing her activities of daily living without pain or loss of function.
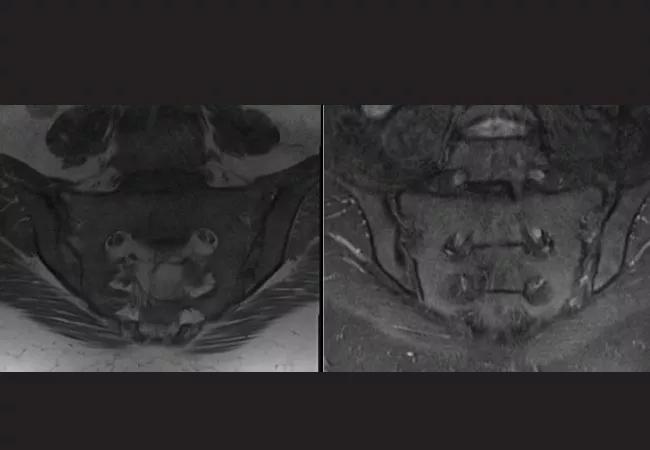
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/5e77918f-cb22-4bf3-b4fd-6e4c5339d3de/22-RHE-3091666-CQD-650x450-Elghawy-1_jpg)
MRI of a former gymnast’s pelvis in coronal oblique views demonstrate sacroiliitis in T1 (left) and STIR (right).
Video content: This video is available to watch online.
View video online (https://www.youtube.com/embed/cqZ4dn-oSP4?feature=oembed)
Athletic Rheumatism: College Wrestler with Knee Pain
A 22-year-old male presented to Cleveland Clinic’s Arthritis and Musculoskeletal Center with left knee pain and swelling. The patient was an in-season college wrestler on holiday break. He reported that three days ago, he developed sudden-onset left knee pain, swelling, redness and difficulty in flexing or extending the knee. He denied any inciting event, trigger or injury. He had not taken any medications for relief, and had tried to ice, although he noted that even touching the knee was exquisitely painful. He noted that he had similar symptoms two months ago that resolved on their own after a few days with ibuprofen.
Advertisement
The patient denied any fever or chills. Interestingly, he noted that he had had a similar episode of pain in his left first toe last year that he attributed to “turf toe.”
On exam, the knee was diffusely tender to palpation, warm and erythematous, and had evidence of effusion. There was difficulty flexing the knee beyond 80 degrees because of pain, and the patient was unable to tolerate provocative exams to test for ligamentous derangement.
A knee radiograph was unremarkable, and musculoskeletal ultrasound demonstrated a moderate knee effusion. The knee was aspirated, yielding 34 cc of cloudy, turbid synovial fluid. Fluid analysis demonstrated < 2,000 RBC/uL, 35,616 total nucleated cells/uL with 76% neutrophils, negative Gram stain and culture, and presence of intracellular monosodium urate crystals. A serum uric acid level of 7.4 mg/dL was noted.
Upon further questioning, the patient admitted that he had difficulty reaching his desired weight for his weight class in wrestling and was taking furosemide in an effort to reach that weight. He had obtained this from other members of his team and said he used it last year as well.
The patient was placed on oral colchicine for his gout flare, with complete resolution of his symptoms. Prompt discontinuation of furosemide was advised, and the patient was counseled that if he develops frequent flares, urate-lowering therapy could be considered. Radiographs of his feet did not demonstrate any erosive changes, but it was discussed that his previous history of “turf toe” may have actually been a gout flare.
Advertisement
Competitive athletes are typically highly motivated and adherent to advice and treatment plans formulated by the medical team. Often this is in line with their goals of a quicker recovery and return to sport. But the road to recovery can be impeded – sometimes even misdirected – with a wrong turn, leading to treatment delay and potentially more harm.
In the first case, a former gymnast with a previous low back injury in her teenage years was successfully managed conservatively. Understanding that spondylolysis is a common hyperextension injury in gymnasts is vital in noting that her current complaint started without any new injury. Recognizing that her pain was present in a different location than what was previously reported should prompt a search for an alternative diagnosis.
From a rheumatic perspective, she is well within the age range for inflammatory spondyloarthropathy, and this is further supported by her physical exam, laboratory findings and imaging results. For the patient’s part, a previous injury that was once successfully treated tends to impart confidence that repeating the same treatment plan will fix the issue once again. This can lead to a delay of diagnosis and, ultimately, a slow functional decline that can be debilitating not only to the athlete’s physical well-being, but their personal identity as a competitive athlete.
In the second case, an active, competitive wrestler sought out diuretic therapy in an attempt to lose weight so he could compete in his desired weight class. Wrestlers are under immense stress to compete at the lowest possible weight class they can manage. Unfortunately, this can lead some wrestlers to seek means that are not only illegal in their sport but dangerous to their overall health.
Advertisement
It is well documented that diuretics like furosemide can induce hyperuricemia by increasing urate reabsorption via volume contraction. In a patient like this, who already has a family history of gout, there is a strong predisposition for the personal development of hyperuricemia, likely unmasked even earlier in his life due to diuretic use.
It is important to discuss the effects of improper medication use, as well as the long-term sequelae of uncontrolled crystal arthropathy so that the patient is able to not only compete safely and ethically during his athletic career, but also develops an understanding that his choices today can have serious consequences for his health and well-being long after his career has ended.
Advertisement

The case for continued vigilance, counseling and antivirals

High fevers, diffuse rashes pointed to an unexpected diagnosis

No-cost learning and CME credit are part of this webcast series

Summit broadens understanding of new therapies and disease management

Program empowers users with PsA to take charge of their mental well being

Nitric oxide plays a key role in vascular physiology

CAR T-cell therapy may offer reason for optimism that those with SLE can experience improvement in quality of life.

Unraveling the TNFA receptor 2/dendritic cell axis