Patient’s 2-year symptom history leads to an uncommon diagnosis
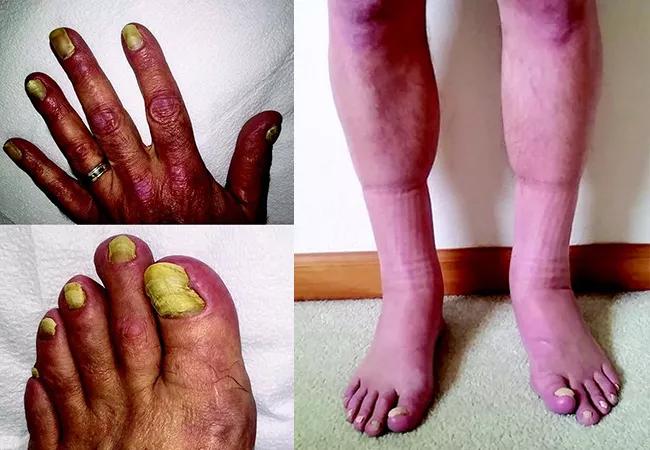
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/124823f2-f3d0-4491-8843-ca16e08e2203/22-RHE-3430660-CQD-650x450-1_jpg)
yellow nail syndrome
By Soumya Chatterjee, MD, MS, and Elliott Chandler Dasenbrook, MD, MHS
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
For two years, a patient with a history of hypertension and obstructive sleep apnea also has been experiencing a variety of new symptoms: nasal congestion, dripping and cough, and thickening and yellow discoloration of his fingernails and toenails. The concurrence of these symptoms points to a rare condition with no known cause.
However, a thorough history, physical examination, and laboratory exams can establish the diagnosis and treatment plan, enabling clinicians and the patient to work together to manage his symptoms.
The 70-year-old patient presents with no fever, a heart rate of 66 bpm, and a blood pressure of 143/72 mmHg. He has no chest pain or joint inflammation. His pulse ox is 97% on room air, and respiration is 18 per minute.
All nails on the patient’s fingers and toes have become brittle, thick and yellow, with some showing distal separation from the nail bed. These changes have been accompanied by a chronic cough and nasal symptoms. Diminished breath sounds are evident upon auscultation, but no crackles can be heard. Cardiac and abdominal examinations are normal.
Lower extremity non-pitting edema and dyspnea have recently developed.
Laboratory tests show normal complete blood count, thyrotropin and comprehensive metabolic panel results. Other results:
Advertisement
A recent chest X-ray to assess his persistent cough did not indicate any obvious cardiopulmonary disease. Electrocardiogram results are normal, although an echocardiogram reveals a pericardial effusion with no evidence of tamponade.
The presence of dyschromic nails, lymphedema and sinus and lung symptoms point to yellow nail syndrome.
With fewer than 400 cases reported so far, yellow nail syndrome is a rare disorder that can affect anyone but typically occurs in men and women 50 and older. Its cause is unknown. It is believed that lymphatic abnormalities lead to the accumulation of lipids which, when oxidized, cause nails to discolor. As a result, longitudinal growth slows, and nails can double in thickness and cause the cuticle and lunula to disappear.
Several more common conditions can cause similar nail symptoms. For example, onychomycosis, especially among adults over 50 – would account for discoloration and thickening, but it could not explain the other symptoms this patient has been experiencing. Psoriasis also can cause changes in nail color and texture; this patient’s other symptoms argue against nail psoriasis.
When yellow nail syndrome is the suspected diagnosis, the next step is to investigate pulmonary manifestations with a thoracic CT scan. This patient’s scan reveals bronchiectasis. Bilateral pleural effusions and a large circumferential pericardial effusion are also present. During thoracentesis, 1400mL of straw-colored fluid is aspirated from the right pleural space. Nonchylous, exudative fluid with a lymphocytic predominance is drained during a pericardial window procedure. Fluid shows no evidence of malignancy; bacterial and fungal cultures are negative.
Advertisement
About 50% of patients with yellow nail syndrome experience spontaneous remission. In the case of this patient, ongoing symptom management is indicated and includes repeated thoracenteses to relieve fluid buildup, manual lymph drainage, and the use of compression stockings for lymphedema. In addition, the patient takes daily vitamin E (1000 IU) and furosemide and is experiencing gradual improvement of symptoms.
Advertisement
Advertisement
Researching the biological basis for why treatment is or is not effective
Scribing system helps create more face-to-face interactions
A conversation with Leonard Calabrese, DO
The case for continued vigilance, counseling and antivirals
High fevers, diffuse rashes pointed to an unexpected diagnosis
No-cost learning and CME credit are part of this webcast series
Summit broadens understanding of new therapies and disease management
Program empowers users with PsA to take charge of their mental well being