Caregivers rely on cross-hospital collaboration to guide critical response
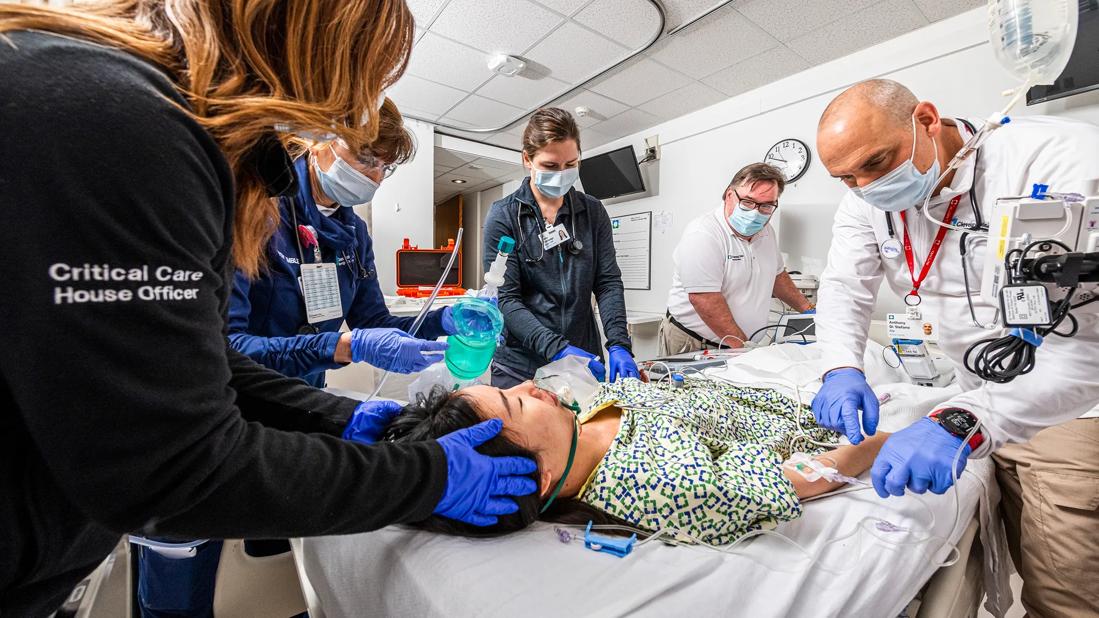
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/91b033ca-1dbe-437c-adf5-a3662c40af9d/NUR_2760508_02-24-22_058_MLC-crop-CQD)
Rapid response team
Seamless coordination is essential when mounting a successful response to cardiac arrests, respiratory failures and other life-threatening hospital emergencies. To minimize confusion and prevent risky time delays, Cleveland Clinic relies on a standardized critical response and resuscitation protocol designed to ensure that all caregivers — regardless of role, shift or location — are aligned in their approach.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
In the event of a hospital “code,” a Rapid Response Team (RRT) is dispatched to the patient's bedside, where specially trained caregivers can conduct a quick assessment, make clinical recommendations and initiate lifesaving interventions. This consistent, organized response is especially important in large hospital systems, where continuity of care can be challenging to achieve across various clinical settings, explains Shannon Pengel, MSN, RN, NE-BC, Vice President, Chief Nursing Officer (CNO) for Cleveland Clinic Main Campus.
“RRTs have enabled us to unify and improve our resuscitation processes by providing a clear roadmap for our clinical teams,” she says. “This standardized approach enables our caregivers to act swiftly and effectively under pressure while building a culture of preparedness and shared responsibility for saving lives.”
Over the course of her 30-year nursing career, Pengel has developed a passion for critical response and resuscitation and continues to find opportunities to share her expertise with her colleagues. Nearly a decade ago, she and Cleveland Clinic anesthesiologist Donn Marciniak, MD, formed a partnership dedicated to improving the institution’s resuscitation response.
“As you can imagine, patient emergencies can create a lot of anxiety and adrenaline,” Pengel says. “It was clear that a standardized RRT protocol would make it easier to reduce treatment gaps, track performance metrics, conduct meaningful debriefs and identify opportunities for further training.”
Advertisement
Encouraged by the success of the institution’s first RRT at Main Campus, the team quickly set out to standardize the resuscitation response enterprise wide. A dedicated Critical Response and Resuscitation Committee has now been established at every Cleveland Clinic hospital. Among the goals of these groups is to ensure that all caregivers have access to well-regulated, state-of-the-art resuscitation equipment.
“We were tasked with ensuring that every patient has access to the same high-quality resuscitation response, regardless of location – and standardization has helped us achieve that mission,” Pengel says.
She adds that errors are minimized when physicians, nurses, respiratory therapists and support staff are trained to follow the same standardized procedures during a code or rapid-response event.
In addition to RRTs, Pengel has helped create dedicated resuscitation-response nursing teams throughout the enterprise. Required to complete ongoing certification and training, these specialists provide resuscitation education, including best practices, to hospital nursing staff and the community.
"The science is constantly evolving, and new resuscitation techniques continue to emerge,” she says. “Patient survival relies on our willingness to stay informed and prepared.”
Pengel emphasizes that every cardiac arrest in a Cleveland Clinic facility is carefully reviewed by the hospital’s Critical Response and Resuscitation Committee. In addition, the health system conducts a separate review of the nursing practices that took place before the critical event “to confirm that our caregivers are doing everything they can to prevent these incidents from happening,” she notes.
Advertisement
Pengel says the data she and her colleagues have accumulated underscores the advantages of having these specialized teams at the bedside. In addition to fostering continuity of care, PPTs enable seamless collaboration between multiple campuses and departments that may have otherwise developed their own “siloed” practices, she notes.
“The value these caregivers provide to patients and frontline staff is consistently proven in the metrics,” Pengel explains. “Because clinical outcomes can be analyzed more effectively when the response structure is consistent, the data we’ve collected has been key to fine-tuning and expanding our resuscitation approach.”
This strategy has helped many Cleveland Clinic hospitals meet the Gold Standard established by the American Heart Association, she notes.
In addition to consulting with Cleveland Clinic hospitals, Pengel and Dr. Marciniak regularly lend their expertise to outside healthcare organizations.
“Other hospital systems are eager to explore best practices and potentially replicate our approach, so our work is far from over,” Pengel says. “I can’t think of a more important way to expand our influence.”
Advertisement
Advertisement
Nurse manager turns a patient safety concern into a data-driven effort to improve protocols and inspire innovation
Nurse draws on frontline experience and an engineering background to develop a new approach to incontinence management
How life experience, storytelling and a passion for service sparked a midlife nursing career
Plastic surgery nurses uniquely help patients meet medical, functional and aesthetic goals
Harnessing digital innovations to enhance nurse confidence and clinical outcomes
Regional organizations collaborate to address nurse faculty shortage
How wellness habits help nurses flourish
Planning continues with critical, patient-focused input from nursing teams