Longer, larger study shows higher hernia rates
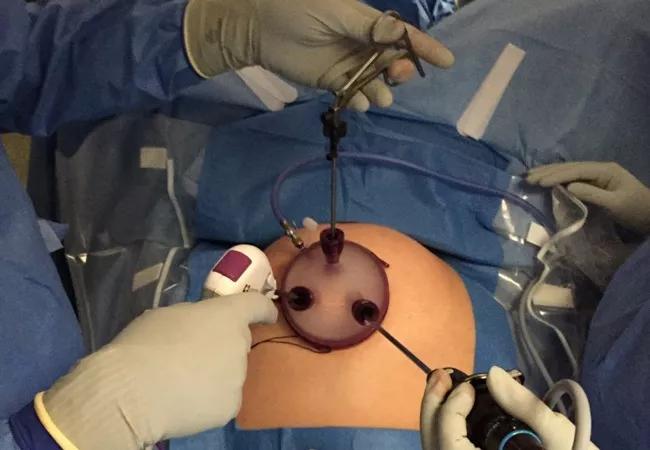
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/c1ce317d-30a3-4673-a5b3-bf279c4049d5/SPL-Hands_650x450_jpg)
SPL-Hands_650x450
Single-port laparoscopic surgery offers a minimally invasive platform for the treatment many gynecological malignancies. The technique allows surgeons to make one incision, typically through the umbilicus, rather than the several incisions used with regular laparoscopic or robotic surgery.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Studies on single-port surgery have shown that it is safe with few complications. However, the current literature is limited by small sample sizes or short follow-up.
Gynecologic oncologist Chad Michener, MD, and colleagues from Cleveland Clinic’s Ob/Gyn & Women’s Health Institute have been utilizing single-port laparoscopy for the management of many gynecologic premalignant and malignant conditions. Dr. Michener and colleagues reviewed their experiences with this surgical platform, focusing on surgical indications, postoperative outcomes and long-term survival information.
Their investigation, published in the American Journal of Obstetrics and Gynecology, demonstrated that single-port surgery has a low rate of adverse short-term outcomes, namely reoperation, surgical-site infection, readmission, intensive care unit (ICU) admission, blood transfusion, conversion to laparotomy and multiport laparoscopy, and venous thromboembolism. When reviewing long-term follow-up, they noticed a 5.5 percent rate of umbilical hernia, higher than reported in previous studies.
“Since we had a three-year follow-up, I think we saw many more hernias than we would have seen in a study with shorter follow-up,” says Dr. Michener, noting that hernia risk has likely been underreported for other types of surgery as well.
The retrospective study included 898 Cleveland Clinic patients who underwent 908 surgeries between 2009 and 2015 with a median follow-up of 37.2 months.
The majority of patients underwent surgery for adnexal masses (36.9 percent) and endometrial hyperplasia/cancer (37.3 percent). Most women underwent hysterectomy (62.7 percent) and removal of one or both fallopian tubes and/or ovaries (86 percent).
Advertisement
The rates of adverse outcomes within 30 days, including reoperation (0.1 percent), intraoperative injury (1.4 percent), ICU admission (0.4 percent), venous thromboembolism (0.3 percent) and blood transfusion (0.8 percent), were low.
The rate of incisional hernia was 5.5 percent, with a mean time-to-hernia development of 570 days. The study identified that in certain patient populations, including those who are obese and who have diabetes, hernia rates approached 23 percent at three years.
Hernia rate may be due to several factors, Dr. Michener notes. The umbilical incision, for example, is somewhat larger with single-port surgery than required in standard laparoscopic surgery. Most commonly, the incision is 15 to 20 millimeters, but sometimes a larger incision is required to remove larger masses and larger uteruses.
The type of surgical closure may also impact hernia rates. “We had not altered our closure technique from standard laparoscopy, where larger port sites are closed with a mass closure tie,” Dr. Michener reports. “Initially, we would stitch all tissue layers together as a mass closure with a running suture of 0 polyglactin. We have changed that over the last year and a half.”
Dr. Michener and his colleagues now carefully isolate the fascia—the layer that prevents hernias—detach the base of the umbilicus and use interrupted sutures with a longer delayed absorbable suture.
Dr. Michener’s team is planning a number of additional studies of single-port surgery. The first will assess the value of these techniques in reducing hernia rates.
Advertisement
They are planning to compare outcomes for single-port surgery, laparotomy, standard laparoscopy and robotic surgery for interval debulking in ovarian or fallopian tube cancers.
“We don’t think overall survival will be different between the three procedures,” Dr. Michener says, “but we want to make sure we’re not setting people up for differences in recurrence or differences in long-term survival just by using different platforms.”
Advertisement
Advertisement
Data point to potential for targeted preconception planning
Reproductive psychiatry helps patients balance medication-related risks
Molecular Profiles Help Guide Referral and Care Planning
Hyperthermic intraperitoneal chemotherapy can improve patient outcomes
Leaning into therapies with the strongest evidence
A Q&A with Cleveland Clinic’s board-certified pediatric and adolescent gynecologist
Increasing uptake remains a challenge
Multidisciplinary teams work together in in-situ scenarios