
Minimally invasive approach, peri- and postoperative protocols reduce risk and recovery time for these rare, magnanimous two-time donors

Minimally invasive pancreas-kidney replacement reduces patient’s pain, expedites recovery

Highlights and insights from recent Cleveland Clinic experience

First-ever procedure restores patient’s health
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
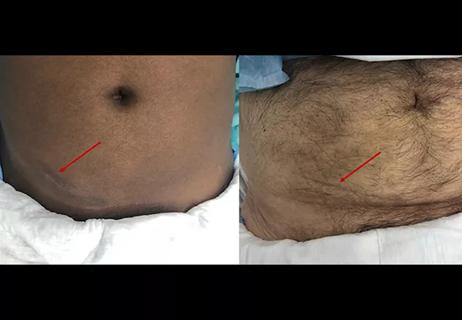
Smaller incision may lead to reduced postoperative pain for some patients

Long-term lung allograft outcomes clinically unaffected by organ exposure, study finds
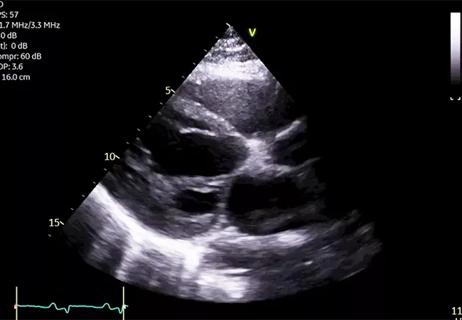
Young man saved multiple times by rapid collaborative response
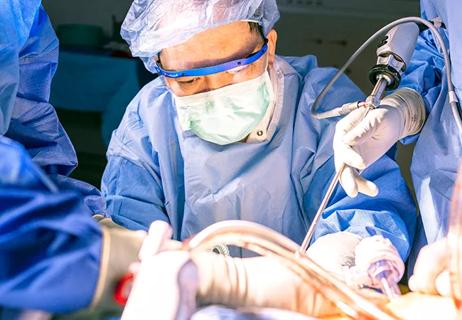
Improving access to lifesaving kidney transplant

Program expands as data continues to show improved outcomes
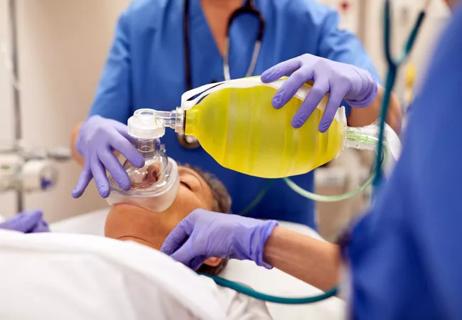
Survey gauges caregivers’ knowledge, opinions about ‘full code’ requirements
Advertisement
Advertisement