Network proximity and EHR analyses identify diabetes drug as a top candidate for risk reduction
A transcriptomics-based study by Cleveland Clinic researchers in collaboration with colleagues at Northwestern University suggests that metformin is a top repurposable drug candidate for atrial fibrillation (AF). The results — based on application of network-medicine methodologies analysis and analysis of electronic health records (EHR) data — show that the diabetes medication is significantly associated with reduced risk of AF.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“This work is an extension of our genomics research to the bedside, which is needed because no new drugs have been approved for AF in over a decade,” says the study’s senior author, Mina Chung, MD, a Cleveland Clinic electrophysiologist and staff in its Departments of Cardiovascular Medicine and Cardiovascular and Metabolic Sciences. “We harnessed drug-target interactions to assemble a drug-target network, used gene set enrichment analysis to nominate candidate drugs, and performed a large-scale pharmacoepidemiologic analysis to validate metformin as a repurposable drug for AF.”
The researchers hypothesized that an integrative network-medicine approach would enhance candidate drug prioritization for AF. For the study, published in Cell Reports Medicine, they began by harnessing gene expression data from 251 patients to generate an AF genetic expression network or disease module. Subsequently, the researchers identified drug targets from a list of 2,891 FDA-approved drugs and calculated network proximity of drug targets to the AF disease module.
Gene expression data from drug-treated human cell lines were used to further narrow the repurposed drug list. Gene set enrichment analysis identified nine drug candidates, including metformin. Functional testing of metformin in human induced pluripotent stem cell (hiPSC)-derived atrial-like cardiomyocytes (a-iCMs) provided validation of the in vitro drug candidates.
“We posited that if a drug significantly reverses dysregulated gene expression, then such drug has the potential of reversing gene neighborhoods in the AF disease module,” says Jessica Castrillon Lal, the study’s first author and a fifth-year graduate student in Cleveland Clinic’s Molecular Medicine PhD program.
Advertisement
“Looking at overlap between significant genes in the AF cohort and the metformin-treated a-iCMs, we found that metformin induced directional changes in six genes upregulated in AF and two genes downregulated in AF,” notes Dr. Chung.
For the large-scale, population-based validation, the researchers leveraged data collected in the Northwestern Medicine Enterprise Data Warehouse between 2011 and 2021. Five drug cohort comparison analyses were performed, as was propensity score matching for age, sex, race and comorbidities.
“Our analysis of the EHR data showed that metformin was significantly associated with a 52% reduced likelihood of AF compared with the combined drug cohort,” Dr. Chung says. “A subgroup analysis also showed that the effect size for metformin was stronger in women than in men.”
“We can trim 10+ years from the drug development pipeline by starting with already approved drugs and testing them in a very computationally efficient way, such as with artificial intelligence technology,” says co-author Feixiong Cheng, PhD, associate staff in the Genomic Medicine Institute in Cleveland Clinic’s Lerner Research Institute.
This work is related to a $14.2 million grant from the National Institutes of Health recently awarded to Dr. Chung and Cleveland Clinic colleagues to investigate new AF treatments using genomic data, as covered previously on Consult QD. According to the authors, a strength of the study is its use of a Cleveland Clinic biorepository of left atrial tissue from a cohort of patients with AF and control individuals to generate the AF disease module, in contrast to traditional disease-associated gene approaches reported in the literature.
Advertisement
Several previous studies have provided strong evidence for an association between AF and metabolic syndrome diseases, and this new research suggests there may be therapeutic benefits to managing metabolic and inflammatory pathways in patients with AF.
“Our group has a significant interest in upstream therapies for AF,” says Dr. Chung. “We need randomized trials to determine whether controlling comorbidities such as obesity, hypertension, heart failure and diabetes improves AF, and whether the drugs for those conditions have a direct effect on AF.”
“We now have many tools to better understand the biological basis of diseases, which allows us to repurpose effective drugs to prevent disease progression,” notes W.H. Wilson Tang, MD, a Cleveland Clinic cardiologist with appointments in the Department of Cellular and Molecular Medicine and the Genomic Medicine Institute in Cleveland Clinic’s Lerner Research Institute. “Metformin is a good example,” says Dr. Tang, who was not involved in the current study. “Not only does it tackle metabolic dysregulation, but it also acts on many aging-related disease processes. However, prospective clinical studies are still needed for scientific validation and clinical adoption.”
The Cleveland Clinic research team led by Dr. Chung is currently enrolling patients in the TRIM-AF trial, a prospective 2×2 factorial study comparing metformin (up to 750 mg twice daily) and/or lifestyle/risk factor modifications for reducing AF burden and progression. The secondary aim is to determine clinical, genomic and biomarker predictors of AF progression that may be used to personalize upstream therapies.
Advertisement
To be eligible, participants must have implanted pacemakers or defibrillators with atrial leads and at least one ≥ 5-minute episode of AF over the prior three months. Randomization is stratified by pacemaker versus implantable cardioverter-defibrillator and rhythm at enrollment (sinus rhythm/atrial paced vs. AF).
When asked about future avenues for research in AF, Dr. Chung says that “with support from the NIH, we will be layering additional omics onto our analyses to further refine the list of candidate drugs for incident AF. We also want to try to identify candidate drugs to slow the progression of AF. Teasing out those types of effects in electronic health record data will be more difficult.”
Advertisement
Advertisement

LAA closure may be compelling option in atrial fibrillation ablation patients at high risk of both stroke and bleeding

UK experts compare and contrast the latest recommendations

While results were negative for metformin, lifestyle counseling showed surprising promise

Investigational pulsed-field ablation system also yielded procedural efficiencies
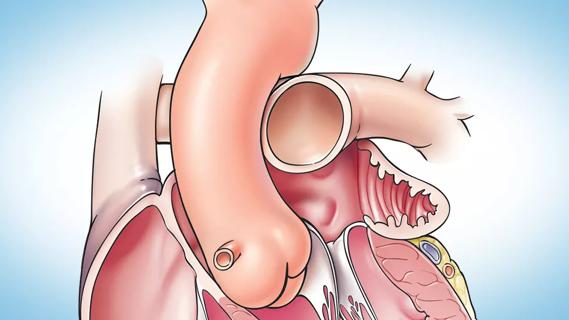
Concomitant AF ablation and LAA occlusion strongly endorsed during elective heart surgery
ACC/AHA panel also upgrades catheter ablation recommendations
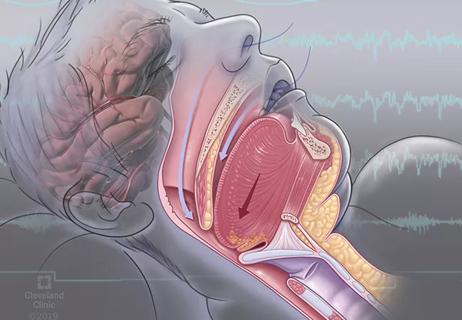
For the first time, risk is shown after accounting for underlying contributions of pulmonary disease

Retrospective analysis finds “hypoxic and sleepy” subtype to confer greatest risk