Expert insights
Juvenile idiopathic arthritis (JIA) and systemic lupus erythematosus (SLE) are common pediatric rheumatologic conditions that manifest with inflammatory arthritis. However, inflammatory arthritis can also be a consequence of infection or a sign of other diseases, such as inflammatory bowel disease (IBD). Establishing the diagnosis of arthritis and finding out the underlying cause can be a challenge in young patients and early-stage disease.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
In this Q&A with Consult QD, Sirada Panupattanapong, MD, Pediatric Rheumatologist in Cleveland Clinic’s Center for Pediatric Rheumatology and Immunology, discusses the utility of ultrasound as a diagnostic tool in pediatric rheumatology.
What is the typical situation that might prompt the use of ultrasound in pediatric rheumatology?
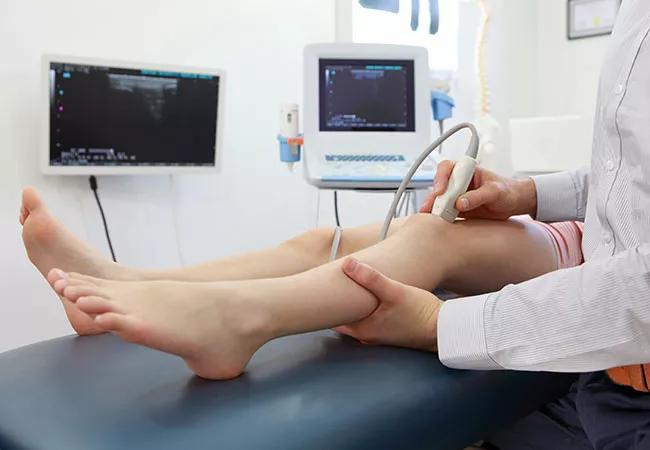
Pediatric patients are typically referred to pediatric rheumatology by their pediatrician to determine the etiology of their joint pain. The major concern is whether the joint pain is caused by arthritis or not. Practically, we can diagnose arthritis by taking the patient’s history and performing physical examination to look for warm swollen joints, tenderness or limited range of motion. However, those signs can be challenging to discern in young children due to small joint size and subcutaneous fat. In situations where physical findings are indefinite, ultrasound is a valuable tool to increase diagnostic accuracy.
How can ultrasound technology help detect changes and inflammation in tissues characteristic for pediatric rheumatologic conditions?
Ultrasound is very useful in examining the structures inside and around the joints. It provides high resolution imaging in the evaluation of arthritis and allows us to see pictures of inflammation of the joint lining (the synovium) and accumulation of fluid inside the affected joint(s). Signs of tendon inflammation are sometimes subtle and difficult to determine by physical exam. Certain types of JIA can involve only the tendons, which is when ultrasound is especially useful. Active inflammation can be detected by using Doppler to look for increased blood flow to the structure.
Advertisement
In which rheumatologic conditions is ultrasound useful?
It is useful in diagnosing any type of inflammatory arthritis due to an underlying medical condition that may or may not be rheumatologic in nature. For example, we can use it in arthritis caused by lupus, IBD (such as Crohn’s disease and ulcerative colitis), or transient inflammatory arthritis due to viral or bacterial infection. An estimated 20 percent of patients with IBD will have some degree of joint involvement.
Ultrasound can demonstrate crystal deposition in gout and pseudo-gout, and osteophyte in osteoarthritis which are common conditions seen in adult patients. In addition to joint structures, utility of ultrasound has been expanded to other conditions including Sjogren’s syndrome — by looking for inflammation in parotid gland, and morphea — by measuring the depth of affected skin and sign of inflammation.
Moreover, in children who undergo steroid joint injections to treat their arthritis, the procedure can be done more safely and accurately under ultrasound guidance as we can see where the needle tip is going. We can maximize the treatment efficacy and minimize the chance of local side effects such as skin hypopigmentation or subcutaneous atrophy at injection site.
Is ultrasound useful in differentiating between the underlying medical conditions that cause arthritis?
Ultrasound can confirm the presence of inflammation in the joint(s) and the number of joints affected by arthritis. Together with the patient’s medical history, physical exam and laboratory test findings, this information can help increase the accuracy of diagnosis. Ultrasound can also help differentiate between the different types of JIA that are characterized by varying extent of joint and tissue involvement — oligoarticular JIA (four or fewer joints affected), polyarticular JIA (five or more joints affected), enthesitis-related arthritis (characterized by inflammation of tendon insertion points) and psoriatic arthritis which is characterized by the varying degree of tendon and joint involvement.
Advertisement
It can also assist us in choosing the best management approach — if few joints are involved such as in oligoarticular JIA, then we would treat the patient with corticosteroid joint injections, but if more than five joints are involved then we would opt for systemic therapy.
What are the advantages of ultrasound compared to other diagnostic methods?
Ultrasound has multiple advantages — we can assess multiple joints in a single exam and perform the exam immediately, on site, and the patient’s family can receive feedback promptly after the exam. Furthermore, it can be done in children at any age, and is well-accepted even in very young children. Our young patients do not need to undergo sedation for the ultrasound exam like they do for an MRI which takes at least half an hour. Compared to X-ray technology, ultrasound does not expose patients to radiation, and is more sensitive in detecting early disease when visible joint damage and erosions have not yet occurred.
How frequently is this technology used in pediatric rheumatology and does it require specialized training?
The use of ultrasound technology in pediatric rheumatology is on the rise, but currently there aren’t many medical centers that have pediatric rheumatologists specifically trained to perform ultrasound. The advantage of having a physician perform ultrasound is that the physicians are aware of the patient’s medical history and can more closely focus on their pathology and obtain additional views. The use of this technology requires both specialized training and experience; I had the opportunity to complete my ultrasound training as a fellow at Washington University in St. Louis/St. Louis Children’s Hospital and have been certified by American College of Rheumatology (RhMSUS certification).
Advertisement
I perform ultrasound routinely in my practice here at Cleveland Clinic to aid diagnostic accuracy, follow treatment response, and guide steroid joint injection. An advantage of ultrasound I found most rewarding is that it helps increase patients’ and parents’ understanding of their diagnosis by visualizing structures and pathology inside the joints. This has resulted in positive effects on clinical management and patient outcomes.
Advertisement
Advertisement

One pediatric urologist’s quest to improve the status quo

Overcoming barriers to implementing clinical trials

Interim results of RUBY study also indicate improved physical function and quality of life

Innovative hardware and AI algorithms aim to detect cardiovascular decline sooner

The benefits of this emerging surgical technology

Integrated care model reduces length of stay, improves outpatient pain management

A closer look at the impact on procedures and patient outcomes

Experts advise thorough assessment of right ventricle and reinforcement of tricuspid valve