Gains are associated with clinical and biomarker benefits in obstructive HCM
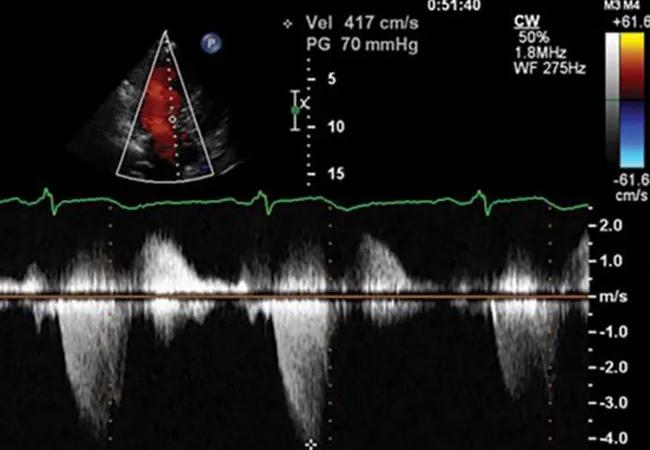
Treatment with the myosin inhibitor mavacamten improves measures of diastolic function in patients with severe symptomatic obstructive hypertrophic cardiomyopathy (HCM) independent of reductions in left ventricular outflow tract (LVOT) gradients and mitral regurgitation.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
So finds a subanalysis of the phase 3 VALOR-HCM study, which previously showed that the novel drug therapy reduced patients’ need for invasive septal reduction therapy. The new subanalysis, published in Circulation: Cardiovascular Imaging, also demonstrated that diastolic improvement correlated with gains in New York Heart Association (NYHA) class, quality-of-life measures and cardiac biomarkers at 16 weeks.
“Clinical improvement with mavacamten appears to be partly mediated by improved diastolic function,” says Cleveland Clinic cardiologist Paul Cremer, MD, MS, first author of the substudy. “This finding has important implications for the use of diastolic assessment to determine prognosis, evaluate treatments and study in other conditions.”
VALOR-HCM is a double-blind, randomized, placebo-controlled crossover VALOR-HCM trial conducted at Cleveland Clinic and 19 other U.S. sites to evaluate mavacamten’s effects among 112 patients with obstructive HCM. All patients had severe symptoms despite maximally tolerated medical therapy and had been referred for septal reduction therapy.
Results after 32 weeks of the trial were recently published online in Circulation and summarized in a prior Consult QD post. Most notably, more than 85% of patients no longer met guideline criteria for septal reduction therapy after mavacamten therapy. The treatment also reduced LVOT gradient and improved clinical function (reduction of ≥ 1 NYHA class) in 90% of patients at 32 weeks. A long-term extension of the trial is ongoing.
Advertisement
Based on results from the first 16 weeks of the VALOR-HCM study, the FDA approved mavacamten (Camzyos®) for adults with symptomatic obstructive HCM in April 2022, making it the first medication approved for this indication. The drug selectively inhibits cardiac myosin, decreasing the number of excess myosin-actin cross bridges in heart muscle that lead to hypercontractility. Although mavacamten improves ventricular compliance, an important factor in heart failure in obstructive HCM, its specific effects on diastolic function have not been well studied.
The substudy evaluated 98 patients (51 of whom took mavacamten) from VALOR-HCM who had diastolic dysfunction grade assessment at baseline and week 16. Principal findings of echocardiographic diastolic function parameters over that time period included the following:
Mavacamten-associated improvements in E/e′ ratio and LAVi were independent of LVOT gradient reduction and mitral regurgitation improvement. In addition, decreased average E/e′ ratio was associated with all the secondary clinical and biomarker endpoints in the VALOR-HCM study, including:
Advertisement
Change in LAVi had no significant correlation with improvements in NYHA functional class or change in KCCQ-23 CSS, but weakly correlated with improved NT-proBNP level (r = 0.20, P = 0.04).
Dr. Cremer notes two major conclusions from the study:
As this was a small exploratory substudy, Dr. Cremer emphasizes that its results should be considered hypothesis-generating. He adds that the findings should be confirmed in studies with longer follow-up, and suggests that they also be assessed in nonobstructive HCM and other cardiac conditions.
He highlights two important implications suggested by these findings. “First, average E/e′ ratio may be a preferred surrogate diastology imaging endpoint in future studies of myosin inhibition in HCM,” he says. “Also, changes in average E/e′ ratio should be considered as a preferred diastolic measure to inform prognosis in obstructive HCM.”
“The clinical benefit of mavacamten is likely partially related to improved ventricular compliance, so effective treatments for obstructive HCM should improve diastolic function in addition to relieving LVOT obstruction and reducing mitral regurgitation,” adds VALOR-HCM principal investigator Milind Desai, MD, MBA, Director of Cleveland Clinic’s Hypertrophic Cardiomyopathy Center and senior author of this subanalysis. “This suggests new avenues of investigation for therapy.”
Advertisement
Advertisement

How Cleveland Clinic is using and testing TMVR systems and approaches

NIH-funded comparative trial will complete enrollment soon

How Cleveland Clinic is helping shape the evolution of M-TEER for secondary and primary MR

Optimal management requires an experienced center

Safety and efficacy are comparable to open repair across 2,600+ cases at Cleveland Clinic

Why and how Cleveland Clinic achieves repair in 99% of patients

Multimodal evaluations reveal more anatomic details to inform treatment

Insights on ex vivo lung perfusion, dual-organ transplant, cardiac comorbidities and more