Researching the biological basis for why treatment is or is not effective
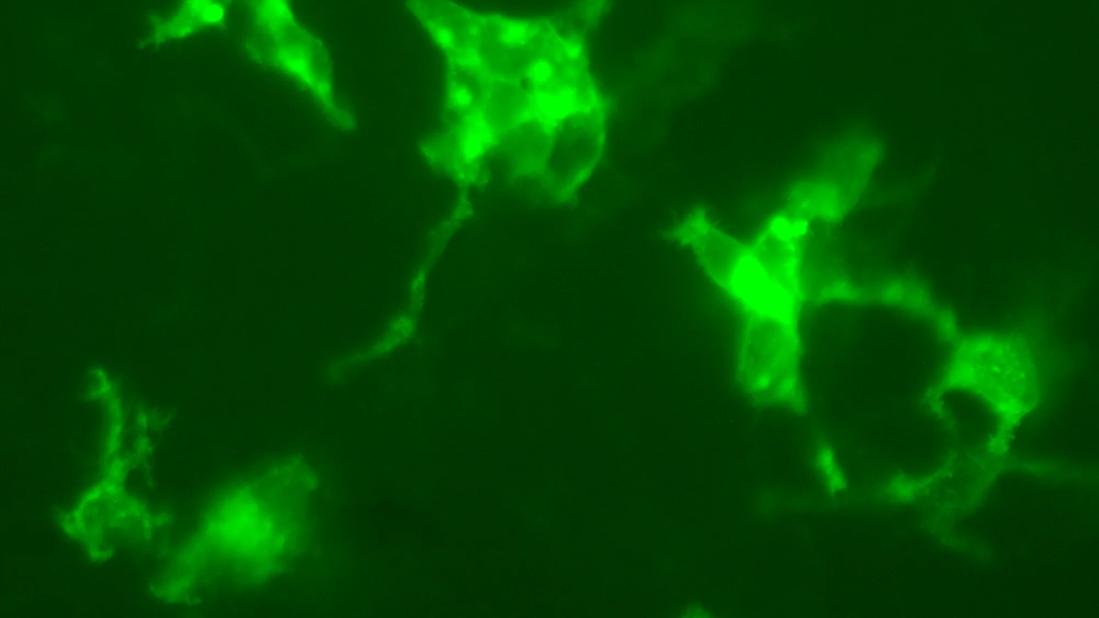
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/36c96bf0-fe93-4cad-b161-b6a87cf6b003/TNFR-inhibitors-husni)
Slide images of membrane of endothelial cells.
By M. Elaine Husni, MD, MPH, Unnikrishnan M. Chandrasekharan, PhD, and Chris Sun, BS
Tumor necrosis factor alpha (TNF-α) inhibitors (TNFi) represent a cornerstone of therapy for psoriatic arthritis (PsA). Yet up to 40% of patients either fail to respond, achieve only partial benefit or lose therapeutic efficacy over time. The biological basis for this variability in treatment response remains poorly understood, and currently no biomarker exists to guide clinicians in predicting who will benefit from TNFi therapy.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Addressing this gap is a major focus of the Elaine Husni laboratory. TNF-α signals through two receptors, TNFR1 and TNFR2. Interestingly, a single nucleotide polymorphism in the TNFR2 gene (rs1061622) has been implicated in TNFi responsiveness across multiple immune-mediated diseases. This polymorphism results in either a methionine (TNFR2-M, the major allele present in ~80%-95% of the population) or an arginine (TNFR2-R, the minor allele present in ~5%-20%) at amino acid position 196. Patients carrying the TNFR2-R variant have been reported to respond less favorably to TNFi therapy. Despite this important association, the mechanistic underpinnings of the reduced responsiveness remain unknown.
To explore this question, we examined whether the TNFR2-M and TNFR2-R variants differ in cellular localization, a factor that could alter receptor availability for TNF-α binding and downstream signaling. Using cultured human endothelial cells, we expressed GFP-tagged TNFR2-M or TNFR2-R and visualized their distribution with fluorescence microscopy. Strikingly, TNFR2-M localized predominantly at the cell membrane, whereas TNFR2-R was largely retained intracellularly.
This difference in receptor trafficking may reduce surface accessibility of TNFR2-R to TNF-α, thereby altering signaling dynamics and ultimately contributing to diminished TNFi responsiveness.
These findings provide a novel mechanistic link between TNFR2 genetic variation and treatment response in PsA. By illuminating how a single amino acid change can influence receptor localization and function, this work highlights a potential pathway for precision medicine approaches in PsA and opens the door to new therapeutic strategies for patients who do not respond to current TNF blockade.
Advertisement
M. Elaine Husni, MD, MPH, is Vice Chair of Rheumatology and Director, Arthritis and Musculoskeletal Center. Lab members Raminderjit Kaur, PhD; Vincent Del Signore, BS; Jean Lin, MD; and Shashank Cheemalavagu, MD, contributed to this research.
Bek, S. et al. Systematic Review: Genetic Biomarkers Associated With Anti-TNF Treatment Response in Infl ammatory Bowel Diseases. Aliment Pharmacol Ther 44, 554-567 (2016).
Canet, L. M. et al. Genetic Variants Within the TNFRSF1B Gene and Susceptibility to Rheumatoid Arthritis and Response to Anti-TNF Drugs: A Multicenter Study. Pharmacogenet Genomics 25, 323-333 (2015).
Gonzalez-Lara, L. et al. The TNFRSF1B rs1061622 Polymorphism (p.M196R) is Associated With Biological Drug Outcome in Psoriasis Ppatients. Arch Dermatol Res 307, 405-412 (2015).
Gottenberg, J. E. et al. Non-TNF-Targeted Biologic vs a Second Anti-TNF Drug to Treat Rheumatoid Arthritis in Patients With Insuffi cient Response to a First Anti-TNF Drug: A Randomized Clinical Trial. JAMA 316, 1172-1180 (2016).
Hetland, M. L. et al. Direct Comparison of Treatment Responses, Remission rates, and Drug Adherence in Patients with Rheumatoid Arthritis Treated With Adalimumab, Etanercept, or Infl iximab: Results From Eight Year of Surveillance of Clinical Practice in the Nationwide Danish DANBIO Registry. Arthritis Rheum 62, 22-32 (2010).
Hyrich, K. L. et al. Outcomes After Switching From One Anti-Tumor Necrosis Factor Alpha Agent to a Second Anti-Tumor Necrosis Factor Alpha Agent in Patients With Rheumatoid Arthritis: Results From a Large UK National Cohort Study. Arthritis Rheum 56, 13-20 (2007).
Advertisement
Xing-Rong, W. et al. Role of TNFRSF1A and TNFRSF1B Polymorphisms In Susceptibility, Severity, and Therapeutic Effi cacy of Etanercept In Human Leukocyte Antigen-B27-Positive Chinese Han Patients With Ankylosing Spondylitis. Medicine (Baltimore) 97, e11677 (2018).
Warren, R. B. et al. Differential Drug Survival of Biologic Therapies for the Treatment of Psoriasis: A Prospective Observational Cohort Study From the British Association of Dermatologists Biologic Interventions Register (BADBIR). J Invest Dermatol 135, 2632-2640 (2015).
Advertisement
Advertisement
Scribing system helps create more face-to-face interactions
A conversation with Leonard Calabrese, DO
The case for continued vigilance, counseling and antivirals
High fevers, diffuse rashes pointed to an unexpected diagnosis
No-cost learning and CME credit are part of this webcast series
Summit broadens understanding of new therapies and disease management
Program empowers users with PsA to take charge of their mental well being
Nitric oxide plays a key role in vascular physiology