Zero cases of structural valve deterioration through latest follow-up
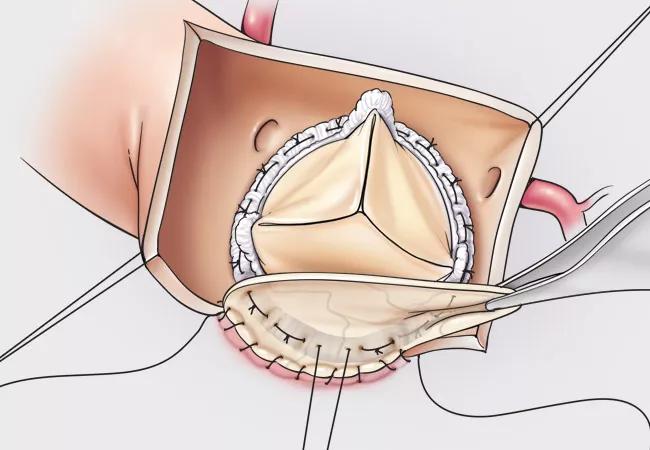
Favorable safety and hemodynamic results with a new tissue valve designed to reduce structural valve deterioration (SVD) in surgical aortic valve replacement (SAVR) continued through five years of follow-up. So reported investigators with the COMMENCE trial at the Society of Thoracic Surgeons (STS) virtual annual meeting in late January.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Moreover, the study valve — a trileaflet bioprosthesis mounted with the bovine pericardial tissue known as Resilia — was associated with no cases of valve thrombosis or SVD through five years.
“These are encouraging findings, because structural valve degeneration is a prime limitation of bioprosthetic valves for younger patients undergoing SAVR,” says COMMENCE co-investigator Lars Svensson, MD, PhD, Chair of Cleveland Clinic’s Miller Family Heart, Vascular & Thoracic Institute. “If these results are maintained through 10 or 15 years, this will be an important development for our younger surgical patients who stand to benefit from a more durable valve. This is particularly the case in view of increasing life expectancy for many patients and a downward trend in the age of patients undergoing SAVR with bioprostheses.”
Bioprosthetic valves hold considerable appeal for younger SAVR patients. In addition to their favorable hemodynamics, they offer freedom from the need for anticoagulation and preserve the option of later transcatheter valve-in-valve interventions as an alternative to reoperation.
At the same time, bioprostheses are vulnerable to calcific degeneration, the most common form of SVD. The various forms of SVD are responsible for as many as 20% of SAVR bioprostheses requiring reintervention within 10 years.
The Resilia tissue technology was designed to reduce calcification. It is also used in the commercially available Inspiris valve from Edwards Lifesciences (covered previously on Consult QD). The bioprosthesis studied in the COMMENCE trial, which is different from Inspiris, has the same design as the Edwards Perimount Magna-Ease valve (3300TFX) except for the addition of the Resilia tissue leaflets.
Advertisement
COMMENCE is a multicenter, prospective, single-arm observational trial with the objective of assessing the safety and efficacy of the Resilia tissue valve. Annual follow-up is being conducted through five years for all patients and through 10 years for a subset of patients.
Overall, 689 adults with aortic valve disease were implanted with the study valve in COMMENCE. Of these, 471 had adequate follow-up for inclusion in the five-year analysis (median, 5 years; mean, 4.3 ± 1.4 years). The remaining enrollees exited the study prior to the five-year visit (n = 153, including 69 deaths) or missed their five-year visit or had a pending five-year visit at the reporting cutoff (n = 37); an additional 28 patients had follow-up beyond 5.5 years and were excluded from the current analysis.
The 471 subjects in the analysis were predominantly men (71.8%) and had a mean age of 66.9 years and a mean STS risk score of 2.0%. Half had New York Heart Association class II symptoms, with approximately a quarter having class I symptoms, another quarter having class III symptoms and a sliver (2%) having class IV symptoms. Concomitant heart procedures were performed along with SAVR in 41% of subjects, but patients requiring emergency or multivalve procedures were excluded from enrollment, as were those with endocarditis. Use of large valve sizes was widespread, with 60% of patients receiving either a 23-mm or a 25-mm valve.
As previously reported by COMMENCE investigators, 30-day mortality and stroke rates were 1.2% and 1.6%, respectively. At five years, freedom from mortality was 89.2% and freedom from stroke was 94.5%. Additionally, at exactly five years 100% of patients remained free from valve thrombosis and from SVD.
Advertisement
Transvalvular regurgitation and paravalvular leak were observed at five years in only 3.7% of and 2.2% patients, respectively, with all cases being mild.
The Resilia valves showed good hemodynamic function as well, with echo-derived mean gradients remaining stable from year 1 (10.2 mmHg) to year 5 (11.5 mmHg) and average effective orifice area holding steady over the same interval (from 1.7 cm2 to 1.6 cm2).
“These intermediate outcomes showing stable gradients, freedom from regurgitation and absence of structural valve deterioration through five years collectively suggest promising durability,” observes Dr. Svensson. “That’s particularly true for the absence of valve deterioration, as all past trials of biological valves have shown the beginnings of structural deterioration by the five-year point.”
He adds that any conclusions about durability must await continued follow-up, however. That will come from the 10-year results in COMMENCE’s extended follow-up cohort as well as from 11-year follow-up in small ongoing RESILIENCE trial.
“If this durability is maintained to 10 years and beyond, the case for SAVR with a biosprosthetic valve in younger patients will be stronger than ever,” Dr. Svensson concludes. “And it will likely fuel interest in testing Resilia tissue technology in TAVR valves as well.”
Advertisement
Advertisement

How Cleveland Clinic is using and testing TMVR systems and approaches

NIH-funded comparative trial will complete enrollment soon

How Cleveland Clinic is helping shape the evolution of M-TEER for secondary and primary MR

Optimal management requires an experienced center

Safety and efficacy are comparable to open repair across 2,600+ cases at Cleveland Clinic

Why and how Cleveland Clinic achieves repair in 99% of patients

Multimodal evaluations reveal more anatomic details to inform treatment

Insights on ex vivo lung perfusion, dual-organ transplant, cardiac comorbidities and more