Markov model simulates patient scenario, explores economy of PRP injections for knee osteoarthritis
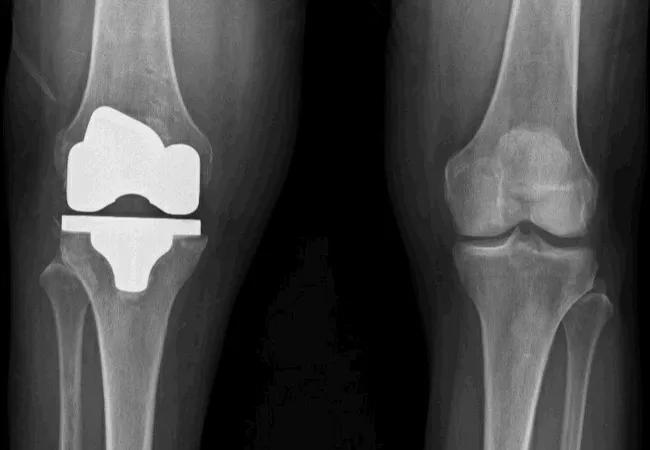
When it comes to the more advanced stages of knee osteoarthritis – and when conservative management has failed – surgical interventions are often utilized. Knee replacements typically provide a predictable outcome, and patients frequently report an improved function and quality of life.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
It’s the earlier stages of disease progression where therapeutic options are less defined, explains Nicolas Piuzzi, MD, an orthopaedic surgeon at Cleveland Clinic.
“This is where we have more questions than answers,” he says. The orthobiologics market has grown considerably over the last decade in response to this unmet clinical need. Platelet-rich plasma (PRP) injections, a concentrated extract of platelets from autologous blood, fall into this category.
When injected into the joint, platelets from autologous blood break down, releasing growth factors, which are believed to decrease inflammation and improve symptoms.
Results from comparative studies tend to favor the utility of PRP injections over other injection therapies, such as steroids and hyaluronic acid. The problem, Dr. Piuzzi explains, is that injection therapies are not structure-modifying. They can help manage symptoms of osteoarthritis, but they don’t alter disease pathology.
Take steroids for example. They are well-utilized, relatively low cost and usually covered by insurance. However, their effect is short-lived, lasting four to six weeks on average. Hyaluronic acid, a gel injection, may or may not be as effective as steroids. There is conflicting evidence about its efficacy. And access is a bit more challenging as it’s only sometimes covered by insurance.
Current literature reports that PRP injections are safe; however, its efficacy is not well-described. Additionally, it is also not covered by insurance. Dr. Piuzzi and a team of researchers at Cleveland Clinic set out to investigate the cost-effectiveness of PRP in delaying the need for total knee arthroplasty (TKA). They reported their findings in The Journal of Bone and Joint Surgery.
Advertisement
The team utilized a Markov model to simulate a patient scenario, intentionally modeling a patient for whom conservative treatments failed. The model represented a 55-year-old patient with Kellgren-Lawrence grade-II or III knee osteoarthritis undergoing a series of three PRP injections with a one-year delay to TKA versus no delay and TKA from the outset. Outcome metrics included total costs and quality-adjusted life-years (QALYs).
Primary findings reveal that from a healthcare payer perspective, PRP injections resulted in 14.55 QALYs compared with that of 14.63 for TKA, with total healthcare costs of $26,619 and $26,235, respectively. TKA was more cost-effective, producing a higher number of QALYs at a lower cost. This was true from a societal perspective as well.
Why compare PRP injections to a well-established and proven treatment? Dr. Piuzzi explains, “Some patients are not ready to have a knee replacement, and it’s reasonable to explore other options with them,” he says. “But this study shows the primary factor preventing PRP injections from being cost-effective is its efficacy, not the cost of the injection itself.”
That’s not to say that PRP injections aren’t a valuable tool for orthopaedists. The study also found that PRP injections are more cost-effective in certain patient subgroups, such as those with a higher risk for perioperative complications. Patients with more comorbidities present higher surgical risk and, as a result, higher costs. In these cases, the use of PRP injections might be cost-effective, even in the current stage of evidence.
Given what is currently known, they may work most favorably as part of a multimodal approach, or for patients who are not candidates for surgery. Dr. Piuzzi says that a randomized controlled trial is the best way to evaluate the efficacy of PRP injections and also identify which patients may benefit most from them. He is currently conducting a randomized controlled trial at Cleveland Clinic to answer these questions.
Advertisement
But determining the economy of PRP injections versus a TKA is an important piece of the puzzle, too, particularly when looking at the bigger picture – the intersection of efficacy, quality of life and healthcare expenditure. “It’s an essential component to consider alongside our active clinical investigations,” he says.
Advertisement
Advertisement

How it’s similar but different from the direct anterior approach

Collaboration must cross borders and disciplines

Systematic review of MOON cohorts demonstrates a need for sex-specific rehab protocols

Should surgeons forgo posterior and lateral approaches?

How chiropractors can reduce unnecessary imaging, lower costs and ease the burden on primary care clinicians

Why shifting away from delayed repairs in high-risk athletes could prevent long-term instability and improve outcomes

Multidisciplinary care can make arthroplasty a safe option even for patients with low ejection fraction

Percutaneous stabilization can increase mobility without disrupting cancer treatment