A Less Morbid Option to Halt Disease Progression
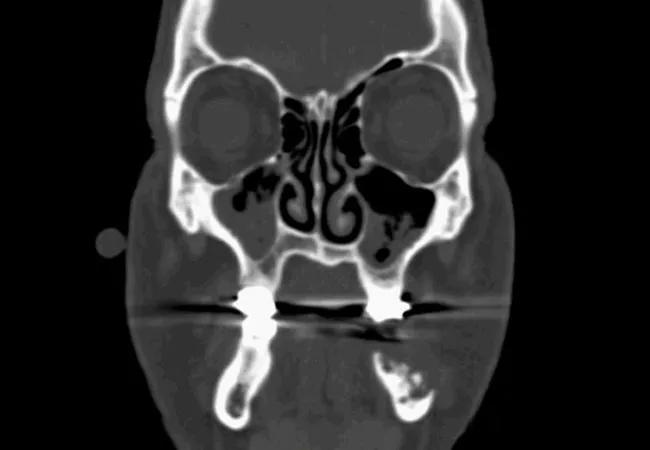
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/1f0ce5af-687f-4658-ab33-d08d5e5286b0/21-HNI-2235264-Fascia-Lata-RescueFlap-Osteoradionecrosis-CQD-hero_650x450_jpg)
Osteoradionecrosis Scan
The anterolateral thigh (ALT) fascia lata (ALTFL) rescue flap is an effective and less morbid intervention in preventing progression of osteoradionecrosis (ORN), according to a study of Cleveland Clinic patients. Results of the retrospective study were recently published in Laryngoscope.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
ORN is a common complication for survivors of head and neck malignancies that significantly impacts quality of life. Current management strategies are usually multimodal and include antibiotics, hyperbaric oxygen (HBO) therapy, selective debridement and additional pharmacological treatment. Refractory cases require repeat therapies and often progress to severe bone destruction which require segmental mandibular resection and reconstruction. To prevent this cascade towards full thickness bone loss, the ALTFL rescue flap imports highly vascularized tissue that acts to improve antibiotic delivery, halt or reverse ischemic changes and provide coverage for exposed bone.
“We have not yet, as a field, established a standard of care in the setting of moderate refractory osteoradionecrosis which can reliably prevent disease progression,” says Michael A. Fritz, MD, Director of the Section of Facial Plastic and Microvascular Surgery in Cleveland Clinic’s Head & Neck Institute and senior author of the paper. “HBO is the current go-to for management, but there’s controversy over how well it works to halt or reverse ORN and more critically, there are no effective options when HBO fails substantial healthy underlying bone is still present. This study helps establish another procedure as a viable and attractive option for patients.”
The procedure involves an isolated transoral technique to elevate compromised mucosa and debride necrotic bone followed by contouring to optimize for vascularized flap coverage. To minimize risk to the remaining viable bone, periosteal elevation is limited to only allow for removal of the compromised bone elements. A fasciocutaneous perforator ALT flap is the harvested from the thigh yielding a thin, highly vascularized sheet. The ALTFL flap is then inset to completely fill the defect and provide coverage for exposed bone with minimal bulk, thus preventing any effects on the airway or oral function. The vascular pedicle is passed through a subcutaneous tunnel and anastomosed with vessels isolated though a minimal access incision. A thin skin graft harvested from the same thigh incision is then sutured over the flap.
Advertisement
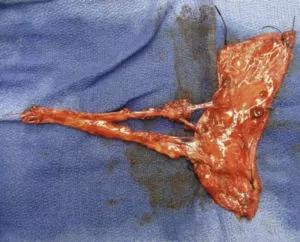
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/3c95aff5-402e-40b3-acf6-00362640db38/21-HNI-2235264-Fascia-Lata-RescueFlap-Osteoradionecrosis-CQD-inset1_800x646-300x242_jpg)
After surgery, patients are able to ambulate and are started on an oral diet that day. The majority of patients are discharged on postoperative day #1 or #2.
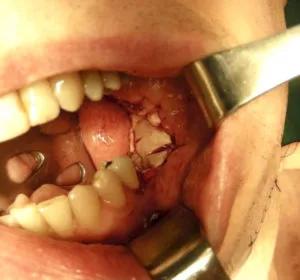
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/feb217ab-89b2-4ced-9138-fe96624937c4/21-HNI-2235264-Fascia-Lata-RescueFlap-Osteoradionecrosis-CQD-inset2_800x747-300x280_jpg)
“We have previously published case studies and data demonstrating the value of this procedure compared with other common approaches, so in this study we wanted to highlight our experience with a larger cohort, multiple sites of ORN reconstruction and a longer follow-up period,” notes Dr. Fritz.
Researchers analyzed data from 23 patients with an average age of 63 years and a total of 24 ALTFL free flap procedures performed by Dr. Fritz between 2011 and 2018. Inclusion required radiographic and clinical evidence of head and neck ORN and either failed HBO therapy or extensive disease unlikely to respond to conservative approaches. Patients were followed for a minimum of one year after surgery.
The most common site of ORN was the mandible (N = 16), followed by the palatomaxilla (N = 4), skull base and cervical spine (N = 3) and valvarium (N = 2). Most recipient vessels were superficial temporal (N = 11) or common facial (N = 10), while angular was used in a few patients (N = 3).
Overall, researchers documented four major complications: unresolved sequelae of ORN requiring fibular free flap (n=1), mandibular fracture with malunion requiring occlusal adjustment (n=1), flap failure with successful follow-up flap (n=1) and recurrent mandibular infection resolved with IV antibiotics (n=1). Four minor complications were noted, including thigh seroma, thigh hematoma and trismus from intraoral scar formation (N = 2). Almost all (95.7%) patients experienced resolution of symptoms and radiographic arrest of ORN and no longer needed antibiotics.
Advertisement
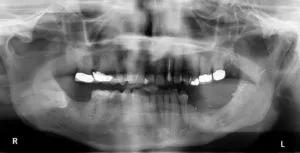
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/8b1b4836-f216-4595-9cd0-2ea811ea7ed2/21-HNI-2235264-Fascia-Lata-RescueFlap-Osteoradionecrosis-CQD-inset3_800x408-300x153_jpg)
“The more we study this procedure, the more promise it shows. The idea is that importing tissue with such robust vascularity reestablishes vascular supply, clears free radicals, helps deliver antibiotics and improves tissue oxygenation,” says Dr. Fritz. “The procedure also allows for reconstruction without risking airway patency or oral motor function, which means shorter hospital stays for patients and less overall financial burden.”
Careful patient selection is key to successful outcomes, he adds. For patients with sufficient, stable bone post debridement, ALTFL is a novel and promising approach to ORN.
Advertisement
Advertisement
Systematic review indicates more can be done for higher-risk patients
Analysis of HNSCC patients shows HPV status to be predictive of higher abundance of oncobacteria within the tumor
Case study illustrates the potential of a dual-subspecialist approach
Evidence-based recommendations for balancing cancer control with quality of life
Study shows no negative impact for individuals with better contralateral ear performance
HNS device offers new solution for those struggling with CPAP
Patient with cerebral palsy undergoes life-saving tumor resection
Specialists are increasingly relying on otolaryngologists for evaluation and treatment of the complex condition