Data system aims to improve orthopaedic care and drive down healthcare costs
Musculoskeletal disorders pose a significant health and economic burden and account for more than half of all chronic conditions in people age 50 or older in industrialized countries. Studies also show $874 billion (5.7% of the GDP) is spent annually in the U.S. on healthcare for patients with musculoskeletal diagnoses. In response, some orthopaedic leaders are calling for greater attention to outcomes research to improve the quality of evidence-based patient care.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Kurt Spindler, MD, Vice Chair for Research in Cleveland Clinic’s Orthopedic and Rheumatologic Institute and Director of the Amy and David Krohn Family Orthopaedic Outcomes Center (OOC), notes that understanding factors that predict poor outcomes is essential to improve and economize care.
“We need to discern between patients who should undeniably proceed with surgery versus those who should consider deferring it until a modifiable risk factor is “corrected,” says Dr. Spindler. “Robust outcomes data will arm us with evidenced-based research that will inform these decisions going forward.”
In 2015, Dr. Spindler piloted what is now the Outcomes Management and Evaluation (OME) system at Cleveland Clinic to collect episode-of-care information and patient-reported outcomes in sports medicine for anterior cruciate ligament repairs and partial meniscectomies. The program, which demonstrated early success, has rapidly expanded since then. As of August 2019, the system has collected patient demographic data, episode-of-care information and patient-reported outcomes, including postoperative pain, function and satisfaction, for over 45,000 unique cases at 16 different Cleveland Clinic hospitals and ambulatory surgery centers.
The initiative has already resulted in nearly 20 research publications — and with almost 40 more active studies. While the earlier publications aim to validate the utility of the system as a research tool, the next wave of studies will start to ask questions of the data, Dr. Spindler says. “It was critical that we first answer the question, ‘Does it work, and is it efficient?’ before we leverage this data to inform point-of-care decisions.”
Advertisement
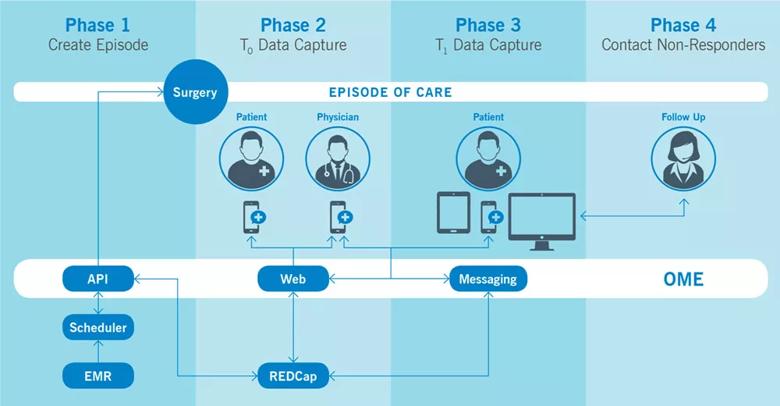
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/afd4879e-ea8b-4ba9-86e7-baf2c64317be/19-ORT-1461-Patient-Data-CQD-Inset_jpg)
Figure. Outcomes Management and Evaluation (OME) system is used across the institution to systematically collect patient-reported outcome measures.
The utility and value of OME is evidenced in rotator cuff repair. Kathleen Derwin, PhD, biomedical engineer in Cleveland Clinic’s Lerner Research Institute and Director of the Musculoskeletal Research Center, recently authored two studies published in the Journal of Shoulder and Elbow Surgery, both stemming from OME data in rotator cuff repair.
The first study demonstrated the validity and efficiency of OME, compared with electronic medical record data, in rotator cuff repair, she says. “Notably, OME had significantly higher data counts for 25% of variables in our analysis,” she says. “We determined OME is a valid tool for further investigations of factors impacting quality and outcomes of rotator cuff repair.”
Taking this one step further, in the second study, co-authored with Eric Ricchetti, MD, shoulder surgeon in Cleveland Clinic’s Department of Orthopaedic Surgery, the team asked a different question of the OME data: What can we learn about how rotator cuff repair surgery is performed in our health system?
The research team found that tear size, a greater number of torn tendons, double-row repair technique and the surgeon were significantly associated with a greater number of anchors used for rotator cuff repair. “This data tell us there is notable variation in surgical techniques when approaching rotator cuff repair,” remarks Dr. Ricchetti. He notes that surveying surgeons about their particular approach, in addition to analyzing patient-reported outcomes one and two years after the surgery, will add insight to this investigation.
Advertisement
Ultimately, this work will help standardize procedures and develop new understandings – in rotator cuff repair and other elective orthopaedic surgeries – as to why some approaches may be more effective for a particular cohort of patients.
Dr. Spindler is eager to continue building the program by expanding into new sites and adding new episodes of care across orthopaedic and nonorthopaedic specialties.
“We’ve already seen a high volume of research activity coming out of the OME,” he says. “We hope to continue engaging more physicians and researchers at different sites to accrue more patient data. We believe this is a real opportunity to personalize orthopaedic care and drive down healthcare costs.”
Piuzzi NS, Strnad G, Brooks P, et al. Implementing a Scientifically Valid, Cost-Effective, and Scalable Data Collection System at Point of Care. The Journal of Bone and Joint Surgery. 2019;101(5):458-464.
BMUS: The Burden of Musculoskeletal Diseases in the United States. BMUS: The Burden of Musculoskeletal Diseases in the United States. https://www.boneandjointburden.org
Advertisement
Advertisement

How it’s similar but different from the direct anterior approach

Collaboration must cross borders and disciplines

Systematic review of MOON cohorts demonstrates a need for sex-specific rehab protocols

Should surgeons forgo posterior and lateral approaches?

How chiropractors can reduce unnecessary imaging, lower costs and ease the burden on primary care clinicians

Why shifting away from delayed repairs in high-risk athletes could prevent long-term instability and improve outcomes

Multidisciplinary care can make arthroplasty a safe option even for patients with low ejection fraction

Percutaneous stabilization can increase mobility without disrupting cancer treatment