Resourceful nurses devise timely safety solutions
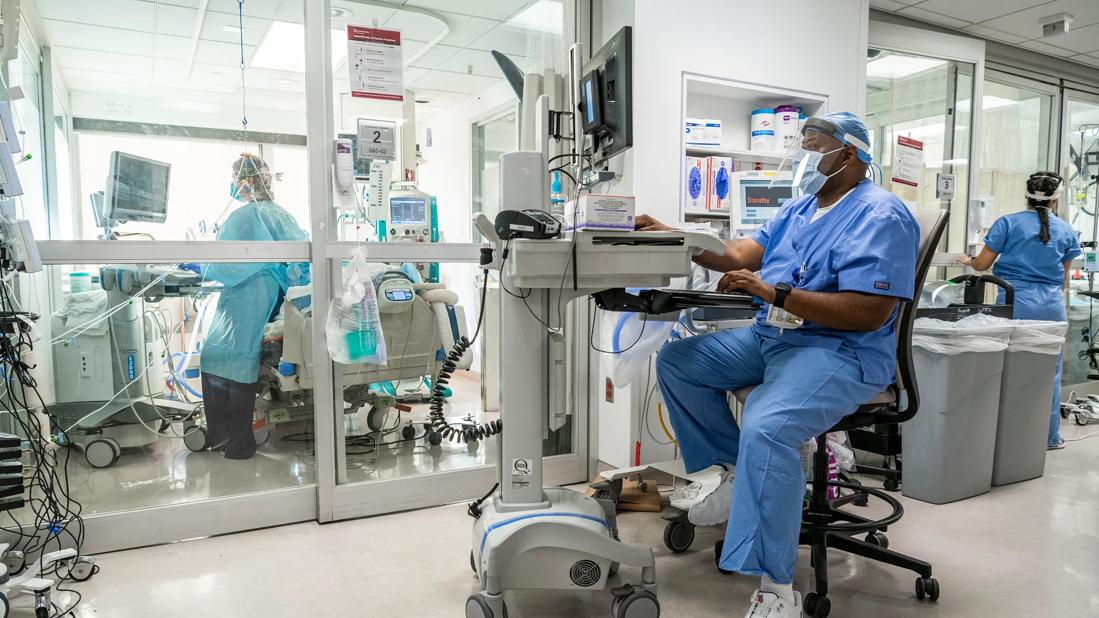
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/89d791d0-9796-4c67-8f18-65750dc23905/HRC_1959003_11-12-20_0707_MLC-jpg)
20-NUR-2036323-PandemicFastTracksInnovations-CQD_650x450
At the start of 2020, nurses were using an average of 66 pieces of personal protective equipment (PPE) each day when entering COVID-19 patient isolation rooms in the intensive care units. Soon into the pandemic, Cleveland Clinic nurses began using the buddy system to put on and take off personal protective equipment.
That was one among a number of innovations last year that allowed Cleveland Clinic nurses to excel during the global health crisis. (Another was the High-Line, a system to raise IV tubing off the floor of patient rooms.)
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Together with infection prevention experts, nurses in the neurological and medical intensive care units developed the PPE buddy system, putting steps in place for nurses to collaborate when they don and doff all PPE needed for entering a patient room.
Video tutorials and visual guides helped make the procedure understood by all, says Terri Murray, MSN, RN, NEA-BC, Nursing Director for the Respiratory Institute, the Head & Neck Institute and Infectious Disease, Main Campus.
Before a nurse enters a patient room, their buddy is on hand to help don equipment to cover their body, eyes and mouth. Physicians also adopted this interdisciplinary practice, and it has become part of the culture in the ICUs.
“We wanted to make sure there were no shortcuts when putting on personal protective equipment, and that there was minimal risk of contamination of personal protective equipment and each other,” Murray says. “We used algorithms and a picture board to enculturate the process, and nurse managers stressed its importance.”
Myra Cook, DNP, APRN, ACNS-BC, clinical nurse specialist in the Cardiovascular ICU, says the buddy system became a best practice for nurses. It proved particularly helpful as safety protocols were refined during the rapidly evolving pandemic.
“There were so many iterations of personal protective equipment due to emerging knowledge and the need, for example, to reuse N95 masks,” says Dr. Cook. “Nurse leaders had to regularly update clinical nurses on revised protocols related to the best steps of donning and doffing.”
Advertisement
Teaming up with a buddy helped ensure that nurses followed protocol, curbed infections and remained safe.
Advertisement
Advertisement
Veteran nurse shares how perseverance and support can fuel impactful ideas
Interdisciplinary initiative leverages technology, documentation and diagnostic clarity to prevent skin breakdown
Program helps caregivers prepare for the unique pressures of the ICU
Multidisciplinary simulations provide realistic emergency training to help achieve optimal patient outcomes
How critical care expertise, rapid decision-making and patient advocacy are shaping perioperative care
Survey identifies opportunities for further training and ongoing moral support
Nursing quality experts help drive policies and practices designed to meet the highest clinical standards
Innovative workforce strategy transforms nursing careers through education, flexibility and ongoing support