Similarly, patients with noninfectious uveitis have a higher risk of being diagnosed with an autoimmune disease within five years
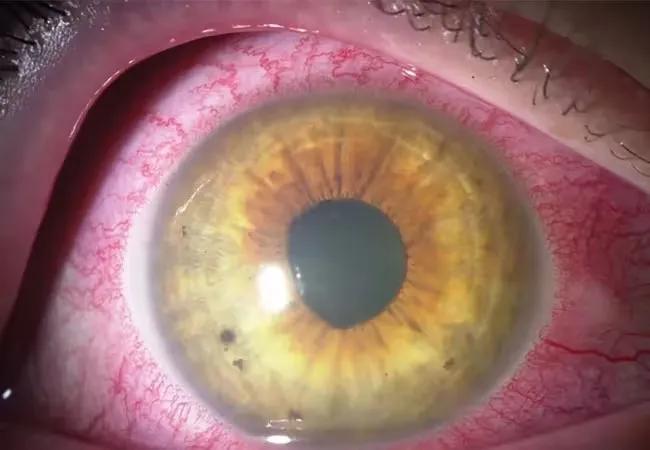
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/9a3eeafb-ddae-4b27-b9e9-5e37a4f454c1/autoimmune-inflammatory-diseases-uveitis)
Eye with inflammation
Patients with ankylosing spondylitis are more than seven times more likely to develop uveitis, reports a new study. Patients with juvenile idiopathic arthritis (JIA) are more than five times more likely to develop the ocular inflammatory condition.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
While an association between immune-mediated inflammatory diseases (IMIDs) and uveitis has long been presumed, the recent study is the first to quantify the risk in 12 different diseases. Researchers also found that patients with new-onset noninfectious uveitis had a higher risk of developing an IMID or already being diagnosed with one.
“We’ve known there’s a correlation between autoimmune diseases and uveitis, but now we better understand the magnitude of correlation,” says senior author Sumit Sharma, MD, a vitreoretinal surgeon at Cleveland Clinic Cole Eye Institute. “All 12 of the IMIDs we studied showed an increased risk of developing uveitis and vice versa, but for some specific IMIDs — including ankylosing spondylitis and JIA — the correlation was remarkable.”
Recognizing the link between IMIDs and uveitis is essential for enhancing early detection, refining treatment approaches and avoiding complications that could jeopardize vision, say the researchers.
The study was made possible thanks to electronic health record (EHR) data from more than 60 U.S. healthcare organizations in a global database.
“Uveitis is relatively rare in the general population, so it’s hard to quantify risk and draw meaningful conclusions based on data from a single institution,” explains Nitesh Mohan, a student at Cleveland Clinic Lerner College of Medicine who was lead author of the study. “Having access to a large EHR database allowed us to identify relationships that we weren’t able to study before.”
Advertisement
The retrospective study published in the American Journal of Ophthalmology used 2006-2025 code data from more than 120 million patients to assess:
In all three analyses, the risk of having or developing comorbid IMID and uveitis was higher than in patients without either an IMID or uveitis, although the risk varied by IMID.
| Risk of uveitis within 5 years of diagnosis (95% CI) | Risk of diagnosis within 5 years of uveitis (95% CI) | Odds of preexisting diagnosis in patients with uveitis (95% CI) | |
|---|---|---|---|
| Ankylosing spondylitis | 7.71 (5.84-10.19) | 15.61 (13.42-18.17) | 38.91 (31.21-48.51) |
| Juvenile idiopathic arthritis | 5.13 (3.51-7.49) | 23.32 (17.52-31.04) | 82.58 (58.59-116.39) |
| Systemic vasculitis | 4.61 (3.73-5.69) | 2.73 (2.42-3.08) | 7.21 (5.73-9.06) |
| Sarcoidosis | 3.67 (3.02-4.47) | 9.99 (8.86-11.26) | 13.83 (12.17-15.71) |
| Giant cell arteritis | 3.24 (2.58-4.07) | 2.39 (2.03-2.82) | 6.06 (4.24-8.66) |
| ANCA-associated vasculitis | 3.18 (1.84-5.48) | 6.74 (4.93-9.22) | 7.72 (5.34-11.16) |
| Scleroderma | 2.52 (1.64-3.87) | 2.12 (1.67-2.70) | 1.71 (1.28-2.29) |
| Rheumatoid arthritis | 2.40 (2.19-2.64) | 2.57 (2.43-2.71) | 2.42 (2.26-2.58) |
| Psoriasis | 2.11 (1.88-2.38) | 1.52 (1.42-1.62) | 1.82 (1.68-1.97) |
| Systemic lupus erythematosus | 2.09 (1.77-2.46) | 2.40 (2.15-2.68) | 2.75 (2.47-3.07) |
| Inflammatory bowel disease | 1.84 (1.62-2.09) | 1.78 (1.64-1.92) | 2.60 (2.40-2.81) |
| Multiple sclerosis | 1.64 (1.36-1.97) | 3.14 (2.76-3.58) | 2.22 (1.99-2.48) |
| Ankylosing spondylitis | |||
| Risk of uveitis within 5 years of diagnosis (95% CI) | |||
| 7.71 (5.84-10.19) | |||
| Risk of diagnosis within 5 years of uveitis (95% CI) | |||
| 15.61 (13.42-18.17) | |||
| Odds of preexisting diagnosis in patients with uveitis (95% CI) | |||
| 38.91 (31.21-48.51) | |||
| Juvenile idiopathic arthritis | |||
| Risk of uveitis within 5 years of diagnosis (95% CI) | |||
| 5.13 (3.51-7.49) | |||
| Risk of diagnosis within 5 years of uveitis (95% CI) | |||
| 23.32 (17.52-31.04) | |||
| Odds of preexisting diagnosis in patients with uveitis (95% CI) | |||
| 82.58 (58.59-116.39) | |||
| Systemic vasculitis | |||
| Risk of uveitis within 5 years of diagnosis (95% CI) | |||
| 4.61 (3.73-5.69) | |||
| Risk of diagnosis within 5 years of uveitis (95% CI) | |||
| 2.73 (2.42-3.08) | |||
| Odds of preexisting diagnosis in patients with uveitis (95% CI) | |||
| 7.21 (5.73-9.06) | |||
| Sarcoidosis | |||
| Risk of uveitis within 5 years of diagnosis (95% CI) | |||
| 3.67 (3.02-4.47) | |||
| Risk of diagnosis within 5 years of uveitis (95% CI) | |||
| 9.99 (8.86-11.26) | |||
| Odds of preexisting diagnosis in patients with uveitis (95% CI) | |||
| 13.83 (12.17-15.71) | |||
| Giant cell arteritis | |||
| Risk of uveitis within 5 years of diagnosis (95% CI) | |||
| 3.24 (2.58-4.07) | |||
| Risk of diagnosis within 5 years of uveitis (95% CI) | |||
| 2.39 (2.03-2.82) | |||
| Odds of preexisting diagnosis in patients with uveitis (95% CI) | |||
| 6.06 (4.24-8.66) | |||
| ANCA-associated vasculitis | |||
| Risk of uveitis within 5 years of diagnosis (95% CI) | |||
| 3.18 (1.84-5.48) | |||
| Risk of diagnosis within 5 years of uveitis (95% CI) | |||
| 6.74 (4.93-9.22) | |||
| Odds of preexisting diagnosis in patients with uveitis (95% CI) | |||
| 7.72 (5.34-11.16) | |||
| Scleroderma | |||
| Risk of uveitis within 5 years of diagnosis (95% CI) | |||
| 2.52 (1.64-3.87) | |||
| Risk of diagnosis within 5 years of uveitis (95% CI) | |||
| 2.12 (1.67-2.70) | |||
| Odds of preexisting diagnosis in patients with uveitis (95% CI) | |||
| 1.71 (1.28-2.29) | |||
| Rheumatoid arthritis | |||
| Risk of uveitis within 5 years of diagnosis (95% CI) | |||
| 2.40 (2.19-2.64) | |||
| Risk of diagnosis within 5 years of uveitis (95% CI) | |||
| 2.57 (2.43-2.71) | |||
| Odds of preexisting diagnosis in patients with uveitis (95% CI) | |||
| 2.42 (2.26-2.58) | |||
| Psoriasis | |||
| Risk of uveitis within 5 years of diagnosis (95% CI) | |||
| 2.11 (1.88-2.38) | |||
| Risk of diagnosis within 5 years of uveitis (95% CI) | |||
| 1.52 (1.42-1.62) | |||
| Odds of preexisting diagnosis in patients with uveitis (95% CI) | |||
| 1.82 (1.68-1.97) | |||
| Systemic lupus erythematosus | |||
| Risk of uveitis within 5 years of diagnosis (95% CI) | |||
| 2.09 (1.77-2.46) | |||
| Risk of diagnosis within 5 years of uveitis (95% CI) | |||
| 2.40 (2.15-2.68) | |||
| Odds of preexisting diagnosis in patients with uveitis (95% CI) | |||
| 2.75 (2.47-3.07) | |||
| Inflammatory bowel disease | |||
| Risk of uveitis within 5 years of diagnosis (95% CI) | |||
| 1.84 (1.62-2.09) | |||
| Risk of diagnosis within 5 years of uveitis (95% CI) | |||
| 1.78 (1.64-1.92) | |||
| Odds of preexisting diagnosis in patients with uveitis (95% CI) | |||
| 2.60 (2.40-2.81) | |||
| Multiple sclerosis | |||
| Risk of uveitis within 5 years of diagnosis (95% CI) | |||
| 1.64 (1.36-1.97) | |||
| Risk of diagnosis within 5 years of uveitis (95% CI) | |||
| 3.14 (2.76-3.58) | |||
| Odds of preexisting diagnosis in patients with uveitis (95% CI) | |||
| 2.22 (1.99-2.48) |
ANCA = antineutrophil cytoplasmic antibody
“We found that ankylosing spondylitis and JIA were the two diseases most closely linked with uveitis,” Mohan says. “Other IMIDs are more closely associated with uveitis than we previously thought. Giant cell arteritis, for example, often has ophthalmic complications, but providers often don’t consider uveitis as one of them. Other diseases, like scleroderma, also typically don’t trigger concerns for uveitis.”
A separate study recently published by Dr. Sharma describes the spectrum of uveitis and retinal vasculitis in a series of patients with systemic sclerosis.
Ophthalmology and rheumatology specialists often work together on patient care. This study highlights just how closely they should be collaborating, say the authors.
“Patients who see a rheumatologist for autoimmune disease may be advised to watch for vision changes or eye symptoms, but it may be more helpful to specify what they’re looking for: flashes, floaters, eye pain and redness, for example,” advises Dr. Sharma. “They also should be alerted to see an ophthalmologist as soon as possible after those symptoms arise, before there’s lasting damage to their vision.”
Advertisement
The same is true for ophthalmologists evaluating a patient with intraocular inflammation or uveitis, he notes. Inquiring specifically about joint pain, skin rashes, fatigue, malaise and headaches can help identify patients who should be referred promptly to rheumatology for assessment of a potential IMID.
“Our study does not necessarily indicate that autoimmune diseases directly cause uveitis or vice versa,” adds Mohan. “However, there appears to be a close association, possibly due to shared pathophysiology like overactivation of the immune system or upregulation of pro-inflammatory cytokines, which can perpetuate both conditions.”
Advertisement
Advertisement
Therapies include steroid implants, immunomodulation and biologics
How to use? Consider starting during the acute attack and seek patient preferences for chronic use
Distinct MRI signature includes lesions beyond the corpus callosum, features predictive of vision and hearing loss
Despite less overall volume loss than in MS and NMOSD, volumetric changes correlate with functional decline
It’s time to get familiar with this emerging demyelinating disorder
Early experience with the agents confirms findings from clinical trials
Early data show risk is 73% higher in patients with lupus, 40% higher in patients with rheumatoid arthritis
Despite advancements, care for this rare autoimmune disease is too complex to go it alone