Aggregate data demonstrate a safe and effective treatment for uterine factor infertility
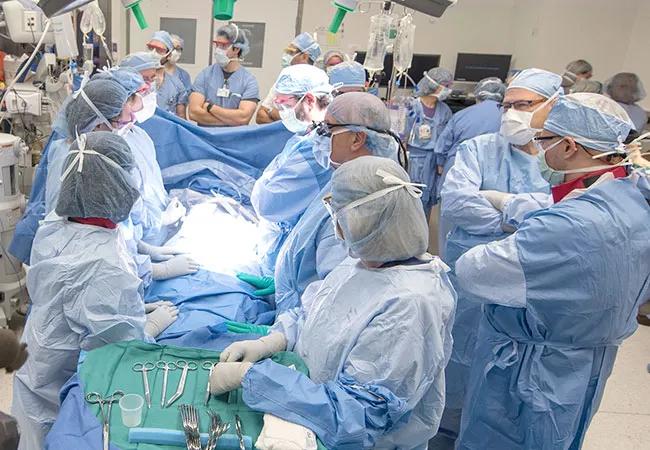
Earlier this month, a woman gave birth to her second child at Cleveland Clinic. While the Cleveland Clinic health system sees more than 10,000 births annually, this particular birth was significant: It marked the fifth child born at Cleveland Clinic from a transplanted uterus – and the first time at Cleveland Clinic that a uterus has had two deliveries following transplantation.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Cleveland Clinic was the first U.S. center to attempt uterus transplantation and has performed eight procedures for patients with absolute uterine factor infertility (AUFI) since the trial began. Together with other pioneering groups in Dallas and Pennsylvania, there have been a total of 33 uterus transplant recipients and over 21 live births.
“Uterus transplantation provides hope for patients who have had few – if any – options for family building. Absolute uterine factor infertility is often a devastating, life-defining diagnosis,” says Elliott Richards, MD. “Absolute uterine factor infertility is not rare. Demonstrating that uterus transplantation is a viable, safe procedure is a necessary first step to expand this life-propagating procedure to benefit even more patients.”
Cleveland Clinic plans to perform 10 transplants for its current trial. To date, four patients have had live births, two have had successful transplants but no live birth yet, two have experienced graft failures and two more transplants are anticipated in the next year. (The program was on hold during part of the COVID-19 pandemic.)
In July 2022, JAMA Surgery published five years of uterus outcome data from Cleveland Clinic, Baylor University Medical Center and the University of Pennsylvania. The study included data on 33 women with AUFI who underwent uterus transplantation between February 2016 and September 2021. Highlights of this report include:
Advertisement
The paper also acknowledges the importance of the United States Uterus Transplant Consortium, which was formed by the three centers in 2019. The consortium has been instrumental in standardizing reporting of outcomes, establishing guidelines for uniform nomenclature, developing novel surgical techniques for deceased donors and fully robotic living donor hysterectomies, allowing early embryo transfer and using the superior uterine veins for graft survival and live birth. “This paper really highlights the collaborative nature of the uterus transplantation centers in the United States, as well as makes a compelling case that uterus transplantation is ready to transition away from a purely investigational era to an emerging efficacious treatment for AUFI,” says Dr. Richards.
Data may be used to counsel women with AUFI on treatment options, as well as help to establish best practices for the development and growth of uterus transplant worldwide. The study also has broader implications. “The uterus is a simply fascinating organ, capable of many astounding feats including cyclic regeneration without scarring and an amazing plasticity to expand to accommodate a full-term pregnancy,” says Dr. Richards. “The first trials were primarily to establish feasibility, safety and efficacy of uterus transplantation, but they pave the way for studies to better understand fundamental aspects of reproductive biology.”
Advertisement
Advertisement

Multidisciplinary teams work together in in-situ scenarios

Uterine transposition cleared the field for radiation therapy

ACOG-informed guidance considers mothers and babies

Prolapse surgery need not automatically mean hysterectomy

Artesunate ointment shows promise as a non-surgical alternative

New guidelines update recommendations

Two blood tests improve risk in assessment after ovarian ultrasound

Recent research underscores association between BV and sexual activity