Study finds broadly similar outcomes between MIS and open surgical approaches
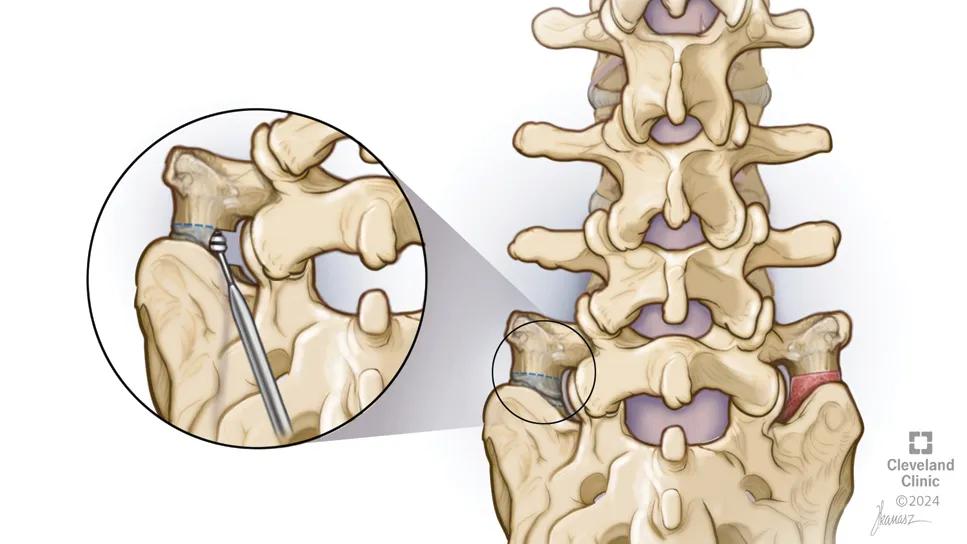
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/cecfa460-41ae-4ea0-b6f2-5e71c1a336e3/lumbar-spine-robotic-screw-illustration)
illustration of lumbar spine with inset showing area of defect
For clinicians treating refractory low back pain, Bertolotti syndrome presents a diagnostic and therapeutic challenge. While many patients respond to conservative management or simple resection, those with concomitant adjacent segment degeneration often require more extensive intervention. A recent Cleveland Clinic study in the Journal of Neurosurgery: Case Lessons (2026;11[8]:CASE25551) provides critical insights for spine surgeons, suggesting that two-level fusion successfully alleviates physical disability in these complex cases regardless of the surgical modality used.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“We found that minimally invasive and robot-assisted techniques offer comparable clinical success to traditional open surgery while significantly improving perioperative efficiency,” says senior and corresponding author Michael Steinmetz, MD, Director of Cleveland Clinic’s Center for Spine Health. “This suggests that the choice of approach can be tailored to patient anatomy and surgeon expertise without compromising functional recovery.”
Bertolotti syndrome is defined by the presence of a lumbosacral transitional vertebra (LSTV) in a patient experiencing localized low back pain. Although LSTVs have been reported in 4% to 36% of the general population, the symptomatic syndrome is far less common. The pain typically originates from the pseudoarticulation between the enlarged transverse process and the sacrum, particularly in types II and IV of the Castellvi classification.
The clinical picture is complicated when patients with Bertolotti syndrome develop severe adjacent segment degeneration. The altered biomechanics of the transitional segment can lead to rapid disc collapse, spondylolisthesis or severe facet arthropathy at the level above the LSTV.
Researchers at Cleveland Clinic’s Center for Spine Health conducted a retrospective review of eight patients who underwent two-level fusion (L4–L5–S1, with one case of L5–L6–S1) for Bertolotti syndrome and associated instability. The cohort was divided into two groups: those receiving open surgery (n = 2) and those undergoing minimally invasive (MIS) or robot-assisted surgery (n = 6).
Advertisement
To determine success, the team used the Patient-Reported Outcomes Measurement Information System (PROMIS) to track physical health, mental health and sleep disturbance. They also used the nine-item Patient Health Questionnaire (PHQ-9) to monitor depression severity. Clinical success was defined by reaching the minimal clinically important difference, which represents a change in status that patients perceive as truly beneficial.
The surgical objective in these cases was to stabilize both the transitional segment and the degenerated adjacent level.
Open approach. Surgery for the two open cases followed standard protocols for transforaminal lumbar interbody fusion (TLIF) and posterolateral fusion (PLF) for L4–S1, including midline incisions, traditional pedicle screw placement, decortication and bone grafting.
MIS and robotic approaches. These procedures were all MIS, with one involving robotic assistance. A TLIF was done at L4–5 and a PLF at L5–S1. Paramedian incisions were guided by computer navigation or robotic arms. Under microscopic visualization, the pseudoarticulation and sacral ala were decorticated using high-speed drills before application of morselized allograft and bone morphogenic protein.
The study revealed that the MIS/robotic procedures were notably faster and involved substantially less blood loss. In the MIS/robotic group, operations averaged 3 hours 30 minutes with median estimated blood loss of 50 mL, compared with 5 hours 49 minutes and 300 mL estimated blood loss in the open surgery group.
Advertisement
Safety and durability were good across the cohort, with no patient in either group experiencing readmission or requiring reoperation over 12-month follow-up.
Radiographic findings demonstrated minimal changes in spinal alignment in both groups. While the open group showed a moderate increase in pelvic tilt, suggesting potential compensation to maintain sagittal balance, both groups maintained appropriate disc heights at the segments above and below the fusion.
From a functional standpoint, both groups improved in physical health at rates comparable to those with more common procedures such as laminectomy. In the MIS/robotic group, 50% of patients achieved the minimal clinically important difference for physical health. Pain scores decreased across the entire cohort, with greater reductions in the MIS/robotic group.
However, the researchers noted a sobering trend regarding mental well-being. Neither approach led to clinically significant improvements in the PROMIS mental health score or the PHQ-9 depression score. In fact, depression severity worsened postoperatively in the open surgery group.
The study authors note that while surgery can effectively repair structural defects and reduce mechanical pain, it may not resolve the complex psychological burden associated with chronic pain syndromes. They advocate for a long-term interdisciplinary care model that includes physical therapy, behavioral health and dedicated pain management to address these nonphysical needs.
The researchers conclude that for surgeons managing Bertolotti syndrome complicated by adjacent segment disease, this study supports a transition toward MIS and robotic approaches when multilevel fusion is indicated. They note that these techniques allow for:
Advertisement
“Spine surgeons must remain selective, however,” Dr. Steinmetz advises. “MIS may not be appropriate for patients with extensive prior spinal surgeries where scar tissue or significantly altered anatomy makes tubular docking or navigation difficult. Furthermore, the choice to move from a one-level fusion to a two-level fusion should be driven by clear evidence of dynamic instability or advanced disc disease at the adjacent level, rather than by symptoms from the pseudoarticulation alone.”
He notes that while the study is limited by its small size — a common issue when researching rare spinal presentation like this — it provides a foundation for future multicenter trials. “Meanwhile,” he concludes, “we have confirmed that two-level fusion is a viable and effective strategy for Bertolotti syndrome with adjacent segment disease. The broadly comparable outcomes between open and minimally invasive techniques allow surgeons to develop individualized treatment plans based on the patient's age, comorbidities and specific spinal morphology.”
Advertisement
Advertisement
Success for these complex operations requires judicious patient selection and presurgical patient optimization
Meta-analyses signal an opportunity to reshape risk stratification and surgical protocols for these comorbidities
Minimally invasive approach is gaining prominence as a fast and safe outpatient procedure
A preview of Cleveland Clinic’s emerging AI platform for spine care decision-making
Opportunities and impacts of a growing surgical approach
Multidisciplinary collaboration is fueling breakthroughs in endoscopic and surgical technology
Join us in Cleveland July 17 for a practical, first-of-kind course
Innovative single-port technique results in no visible scarring