New interventions and policies haven’t increased wait-listing
Access to kidney transplantation today is as limited as it was 20-plus years ago despite numerous efforts to expand it.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
According to a study recently published in the Journal of the American Society of Nephrology (JASN), the rate at which patients with end-stage renal disease (ESRD) were placed on the transplant waitlist was unchanged between 1997 and 2016.
“Access to kidney transplantation has been a problem that has permeated my research career,” says Cleveland Clinic biostatistician Jesse Schold, PhD, lead author of the study. “We’d like to assume that things are getting better, with at least incremental progress over the decades. But the results of this study were striking, showing that we have made no progress at all.”
That’s not to say there hasn’t been ample effort. Numerous policy changes and interventions have attempted to help overcome or sidestep barriers to wait-listing patients with ESRD. While some individual efforts have been promising, their combined effect has been nil.
The JASN study is the first to evaluate the cumulative effect of interventions over an extended period.
“Kidney transplantation has significant benefits for patients with ESRD, including doubling life expectancy and improving quality of life,” says Cleveland Clinic nephrologist Emilio Poggio, MD, senior author of the study. “It also has been shown to reduce healthcare costs when compared to maintenance dialysis.”
To review the long-term pattern of access to this gold-standard treatment, a research team led by Drs. Poggio and Schold studied the U.S. Renal Data System records of 18- to 70-year-olds who were diagnosed with ESRD, were placed on a transplant waitlist or received a kidney transplant between 1997 and 2016. The cohort included more than 1.3 million patients. Researchers assessed time to wait-listing or kidney transplantation from time of diagnosis and found:
Advertisement
One positive finding was that preemptive wait-listing or transplant (prior to starting dialysis) did increase over time, from 5.2% in 1997-2000 to 9.8% in 2013-2016.
“Overall, these results were discouraging,” says Dr. Schold. “Even though many ad hoc interventions have been effective, they haven’t been generalizable, and thus haven’t impacted the broader population.”
The barriers to wait-listing are systemic, says Dr. Schold. The promise of new interventions has been countered by a complex system that involves multiple patient handoffs and requires a higher level of health literacy for patients to navigate the steps for wait-listing.
“This calls for more substantial action that has a more profound effect on our entire system of care,” he says.
The Advancing American Kidney Health Initiative, an executive order issued in 2019 by former President Donald Trump, is a good start. Federal backing to increase transplant accessibility and modernize the transplant program may help move the needle.
Dr. Schold recommends considering an “opt-out” model for transplant referral, at least for patients with ESRD who don’t have contraindications to transplant and likely will meet clinical transplant criteria.
“Instead of requiring a proactive step, referral for evaluation at a transplant center should be automatic — bypassing any barriers inherent in the system,” he says. “Our study included only patients who had been referred for transplant, but there likely were many more who should have been referred but weren’t.”
Advertisement
Advertisement

Milestone minimally invasive surgeries reduce pain and recovery time

Enhanced visualization and dexterity enable safer, more precise procedures and lead to better patient outcomes

Insights on bringing Cleveland Clinic even closer to becoming the best transplant enterprise in the world

Minimally invasive approach, peri- and postoperative protocols reduce risk and recovery time for these rare, magnanimous two-time donors

Minimally invasive pancreas-kidney replacement reduces patient’s pain, expedites recovery

First-ever procedure restores patient’s health
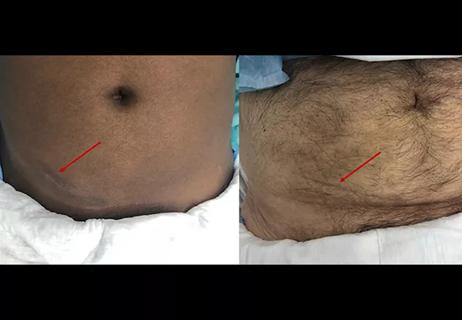
Smaller incision may lead to reduced postoperative pain for some patients
Improving access to lifesaving kidney transplant