Transplant Center makes more organs available to more patients
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
At this moment, more than 114,000 people are waiting for a lifesaving organ transplant. And the longer they wait, the sicker they get. As we strive to be a global leader in saving and restoring lives through transplantation, our goal at Cleveland Clinic is to evaluate patients in need of an organ with efficiency and compassion, and get them on and off that waiting list as quickly as possible.
Putting patients first means figuring out a way to get them the right treatment at the right time – and getting them an organ is absolutely paramount to that.
An enterprise-wide commitment to maximally using every donated organ possible is a piece of what’s driving our success in this endeavor. We are aggressive. We are creative. We are willing to take calculated risks. And we don’t say no easily.
We have been able to cut patients’ wait times by expanding the organ donor pool and making use of less-than-perfect organs. If there is an organ available, we try to find a way to make it work for a patient.
A notable new source of organs is hepatitis C (HCV)-infected livers, kidneys and hearts. Over the course of one year, Cleveland Clinic developed a careful protocol that enables us to offer select transplant candidates who have not been exposed to the virus the option of receiving an HCV-infected organ, which previously would have been undesirable. The availability of highly effective multiple direct-acting antivirals (DAA) that all but cure HCV have made this a reasonable proposition.
Post-transplant, patients are treated with DAA regimens, which appear to have no adverse interactions with anti-rejection medications. The patients clear the HCV and are left with a healthy organ that they wouldn’t have gotten otherwise.
Advertisement
We are also continuing to improve the safety of transplants for living kidney and liver donors. We’ve pioneered techniques that allow us to transplant the smaller left lobe of the liver from a living donor, rather than the larger right lobe. In carefully selected transplants, this minimizes the risk of complications for the donor while producing comparable outcomes for the recipient.
Next in the innovation pipeline is a laparoscopic liver donation technique that we are developing with the potential to cut recovery time, pain and risk for donors. With better safety for living donors, we hope to continue to increase transplant opportunities for healthier patients who are further down the waiting list.
Work is also continuing on an ex vivo organ perfusion device that pumps oxygenated warm blood, nutrients and medication through a donor organ. It can keep a liver alive and functional outside of the body for up to 86 hours and holds the promise of reviving organs that would be rejected for transplant. The perfusion device can also help us assess the function of a donor organ and predict its viability before it’s transplanted. The device is currently in clinical trials.
In many ways, this quest to get the most organs to the most patients is about an attitude. In the intricate world of organ transplant, if you’re always looking for a reason to say no, you will find one for sure. We make a point to not forgo any opportunities we have to say yes – and in return, create more lifesaving chances for patients.
Advertisement
Dr. Miller is Enterprise Director of Transplantation at Cleveland Clinic’s Transplant Center.
Advertisement
Advertisement

Milestone minimally invasive surgeries reduce pain and recovery time

Enhanced visualization and dexterity enable safer, more precise procedures and lead to better patient outcomes

Insights on bringing Cleveland Clinic even closer to becoming the best transplant enterprise in the world

Minimally invasive approach, peri- and postoperative protocols reduce risk and recovery time for these rare, magnanimous two-time donors

Minimally invasive pancreas-kidney replacement reduces patient’s pain, expedites recovery

First-ever procedure restores patient’s health
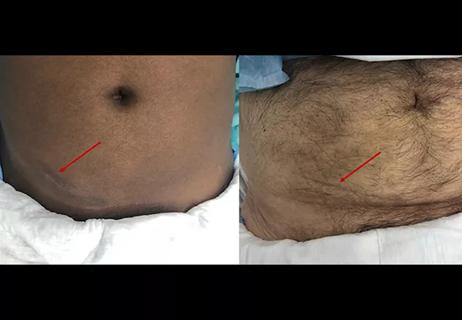
Smaller incision may lead to reduced postoperative pain for some patients
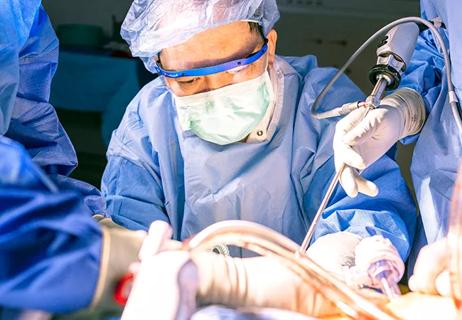
Improving access to lifesaving kidney transplant